Osteoarthritis: Understanding the Causes, Symptoms, and Treatment Options
In this comprehensive article, we will explore the multifaceted aspects of osteoarthritis, a degenerative joint disease. We will delve into its definition, causes, symptoms, diagnosis, treatment options, and prevention strategies. This article aims to provide a comprehensive understanding of osteoarthritis to help individuals better manage and cope with this condition.
1. Introduction
1.1. Definition of Osteoarthritis
Osteoarthritis (OA) is a degenerative joint disease, characterized by the breakdown of cartilage in the joints, resulting in pain, stiffness, and loss of function. As the most common form of arthritis, it affects millions of people worldwide, particularly the elderly population. The disease progresses slowly and typically involves weight-bearing joints such as the knees, hips, and spine, as well as the hands and fingers. In osteoarthritis, the protective cartilage that cushions the ends of the bones gradually deteriorates, leading to joint damage, inflammation, and the formation of bone spurs (osteophytes).
1.2. Prevalence and Impact
Osteoarthritis is a leading cause of disability and reduced quality of life worldwide. According to the World Health Organization (WHO), around 10% to 15% of adults over the age of 60 suffer from some degree of osteoarthritis. The prevalence of OA increases with age and is more common in women than in men, particularly after the age of 50. The disease has a significant impact on individuals, families, and healthcare systems, resulting in substantial costs associated with treatment, loss of productivity, and reduced mobility.
1.3. Importance of Awareness and Education
Raising awareness and providing education on osteoarthritis is crucial in promoting early diagnosis, appropriate management, and prevention strategies. Understanding the risk factors, symptoms, and treatment options can help individuals make informed decisions about their health and well-being. Additionally, public health campaigns and educational programs can contribute to reducing the burden of osteoarthritis on society by promoting healthy lifestyles, early intervention, and better access to healthcare services.
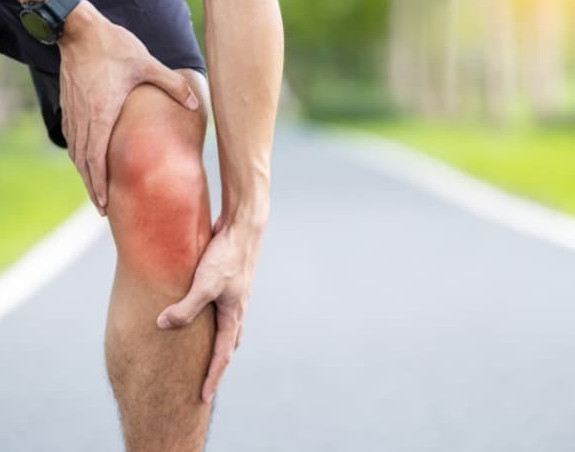
2. Causes of Osteoarthritis
2.1. Aging
Aging is one of the primary risk factors for developing osteoarthritis. As people age, the water content of the cartilage increases, while the protein content decreases. This process results in a reduced ability of the cartilage to resist wear and tear. Moreover, the body’s ability to repair damaged cartilage diminishes with age, leading to the progressive deterioration of joint cartilage and the onset of osteoarthritis symptoms.
2.2. Genetics
Genetics play a role in the development of osteoarthritis. Researchers have identified specific genes associated with an increased risk of developing the disease. Some genes influence cartilage structure and function, while others affect inflammatory processes and pain sensitivity. A family history of osteoarthritis may increase an individual’s risk of developing the condition, suggesting a hereditary component.
2.3. Obesity
Obesity is a significant risk factor for osteoarthritis, particularly in weight-bearing joints such as the knees and hips. Excess body weight puts additional stress on the joints, accelerating the breakdown of cartilage. Furthermore, fat tissue produces inflammatory substances that can contribute to joint inflammation and the progression of osteoarthritis. Maintaining a healthy weight through diet and exercise can help prevent or slow down the progression of the disease.
2.4. Joint Injuries and Overuse
Previous joint injuries or repetitive stress on the joints due to overuse can increase the risk of developing osteoarthritis. Injuries can cause damage to the cartilage or alter the mechanics of the joint, increasing the likelihood of cartilage wear and tear. Occupations or activities that involve repetitive movements, heavy lifting, or high-impact sports can also contribute to joint stress and the development of osteoarthritis.
2.5. Gender
Gender is another factor that influences the risk of developing osteoarthritis. Women are more likely to develop the condition than men, especially after the age of 50. Hormonal changes during menopause may contribute to this increased risk, as estrogen has been shown to have a protective effect on cartilage. Further research is needed to understand the precise mechanisms behind this gender difference.
2.6. Other Contributing Factors
Other factors that may contribute to the development of osteoarthritis include:
- Bone deformities: Some people are born with malformed joints or defective cartilage, which can increase their risk of developing osteoarthritis.
- Metabolic disorders: Certain metabolic conditions, such as diabetes and hemochromatosis (excess iron in the body), can increase the risk of developing osteoarthritis.
- Inflammatory joint diseases: Rheumatoid arthritis, gout, and other inflammatory joint diseases can increase the risk of developing secondary osteoarthritis due to joint damage and inflammation.
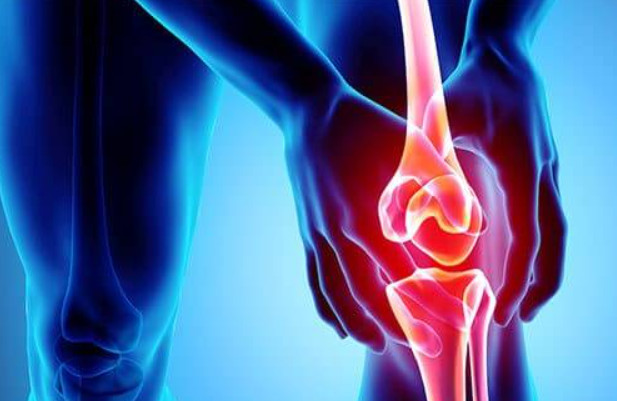
3. Symptoms and Clinical Presentation
3.1. Pain and Stiffness
Pain is the most common symptom of osteoarthritis, typically worsening with activity and improving with rest. Pain may be experienced during joint movement or when pressure is applied to the affected joint. In the early stages of the disease, pain is usually mild and intermittent, but as the condition progresses, it can become more severe and constant. Stiffness is another common symptom, often occurring after periods of inactivity, such as upon waking in the morning or after sitting for an extended time.
3.2. Swelling and Inflammation
Joint swelling is a common feature of osteoarthritis, resulting from the production of excess joint fluid and the formation of bone spurs. Swelling can lead to joint inflammation, causing warmth, redness, and tenderness around the affected joint. This inflammation can further contribute to pain and stiffness, making it difficult to move the joint.
3.3. Loss of Range of Motion
As osteoarthritis progresses, the affected joint may lose its range of motion, making it difficult to perform daily activities. The joint may become less flexible, and individuals may experience limitations in their ability to bend, straighten, or rotate the joint. This loss of range of motion can lead to muscle weakness, reduced mobility, and an increased risk of falls.
3.4. Crepitus and Joint Instability
Crepitus is a grinding or cracking sensation felt in the joint when it is moved, caused by the rubbing of bone against bone as the cartilage wears away. This sensation can sometimes be accompanied by an audible cracking or popping sound. Joint instability is another common symptom of osteoarthritis, as the joint’s supporting structures, such as ligaments and muscles, become weakened, leading to a feeling of the joint “giving way” or “locking up.”
3.5. Joint Deformity
In advanced stages of osteoarthritis, joint deformities can occur as a result of cartilage loss, bone spurs, and changes in the joint’s supporting structures. These deformities can cause the joint to appear enlarged or misshapen, and may further contribute to pain, stiffness, and loss of function.
3.6. Impact on Quality of Life
The symptoms of osteoarthritis can significantly impact an individual’s quality of life. Pain, stiffness, and loss of mobility can make it difficult to perform daily activities, maintain independence, and engage in social or recreational activities. Additionally, individuals with osteoarthritis may experience sleep disturbances due to pain, and may also be at an increased risk of developing depression and anxiety as a result of their chronic pain and reduced functioning.
4. Diagnosis and Assessment
4.1. Medical History
A thorough medical history is the first step in diagnosing osteoarthritis. The healthcare provider will ask about the patient’s symptoms, the onset and progression of pain, any history of joint injuries, and any family history of osteoarthritis. The patient’s age, weight, and occupation may also be relevant factors in assessing the likelihood of osteoarthritis.
4.2. Physical Examination
During the physical examination, the healthcare provider will assess the patient’s affected joints for signs of osteoarthritis, such as swelling, tenderness, warmth, and reduced range of motion. They may also evaluate the patient’s overall posture, muscle strength, and gait to identify any abnormalities that could be contributing to the patient’s symptoms. The healthcare provider may also perform specific tests or maneuvers to evaluate joint stability and to rule out other potential causes of the patient’s symptoms.
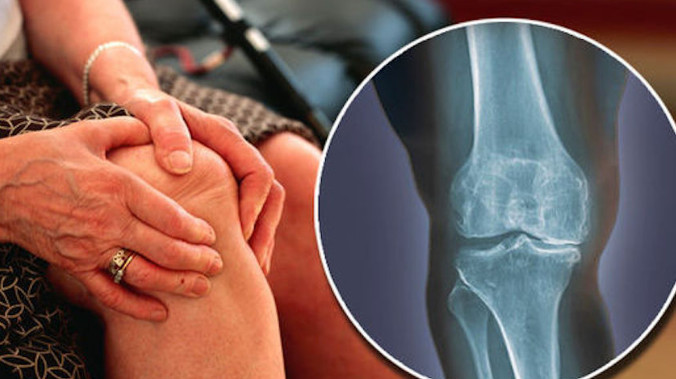
4.3. Imaging Studies (X-ray, MRI, CT scan)
Imaging studies can provide valuable information about the extent of joint damage and help confirm an osteoarthritis diagnosis. X-rays are often the first imaging test used, as they can reveal bone spurs, joint space narrowing, and other characteristic signs of osteoarthritis. However, X-rays do not provide detailed information about the condition of the cartilage, ligaments, and tendons surrounding the joint. Magnetic resonance imaging (MRI) or computed tomography (CT) scans may be ordered to obtain more detailed information about the joint structures and to rule out other potential causes of the patient’s symptoms.
4.4. Laboratory Tests
While there is no specific blood test for diagnosing osteoarthritis, laboratory tests may be ordered to rule out other potential causes of joint pain, such as rheumatoid arthritis or gout. Blood tests can detect inflammatory markers, infection, or other abnormalities that may suggest a different underlying condition. In some cases, the healthcare provider may also order a joint fluid analysis by extracting a small sample of fluid from the affected joint to examine for signs of inflammation, infection, or crystals associated with gout.
4.5. Differential Diagnosis
The healthcare provider will also consider other potential causes of the patient’s symptoms, such as rheumatoid arthritis, gout, tendonitis, bursitis, or joint infections, before confirming a diagnosis of osteoarthritis. The process of ruling out these other conditions, known as the differential diagnosis, is essential to ensure that the patient receives the most appropriate treatment and care for their condition.
5. Treatment Options
5.1. Non-pharmacological Approaches
5.1.1. Physical Therapy
Physical therapy plays a vital role in the management of osteoarthritis, helping to improve joint mobility, muscle strength, and overall function. A physical therapist can design a personalized exercise program that includes range of motion exercises, strengthening exercises, and low-impact aerobic activities to help reduce pain and stiffness, improve joint stability, and prevent further joint damage.
5.1.2. Occupational Therapy
Occupational therapy can help individuals with osteoarthritis adapt to daily activities, minimize joint stress, and improve their quality of life. An occupational therapist can provide recommendations for assistive devices, such as braces, splints, or canes, and suggest modifications to the home or work environment to reduce joint strain and promote safety.
5.1.3. Weight Loss and Diet Modification
Weight loss and maintaining a healthy weight are essential for managing osteoarthritis, particularly for those with knee or hip involvement. Losing excess weight can reduce joint stress, alleviate pain, and improve overall function. A balanced diet that includes a variety of fruits, vegetables, whole grains, lean proteins, and healthy fats can help individuals achieve and maintain a healthy weight, while also providing essential nutrients for joint health.
5.1.4. Assistive Devices
Assistive devices can help individuals with osteoarthritis manage their symptoms and maintain independence. Examples include canes, walkers, braces, or orthotic shoe inserts, which can provide added support, improve joint stability, and reduce pain during daily activities. A healthcare provider or occupational therapist can recommend appropriate assistive devices based on the patient’s specific needs.
5.1.5. Exercise and Physical Activity
Regular exercise and physical activity are crucial for managing osteoarthritis symptoms and promoting overall joint health. Low-impact activities, such as swimming, cycling, or walking, can help improve joint mobility, muscle strength, and cardiovascular fitness, without causing excessive stress on the affected joints. It is important to consult with a healthcare provider or physical therapist before starting a new exercise program.
5.2. Pharmacological Approaches
5.2.1. Analgesics
Analgesics, such as acetaminophen, are often used to manage mild to moderate osteoarthritis pain. These medications provide pain relief but do not have anti-inflammatory effects, and should be used with caution in individuals with liver or kidney problems.
5.2.2. Nonsteroidal Anti-inflammatory Drugs (NSAIDs)
NSAIDs, such as ibuprofen, naproxen, and celecoxib, can help reduce both pain and inflammation in individuals with osteoarthritis. These medications are available over-the-counter or by prescription, but should be used with caution in individuals with gastrointestinal, kidney, or cardiovascular issues.
5.2.3. Intra-articular Injections
Intra-articular injections, such as corticosteroids or hyaluronic acid, can provide temporary relief from osteoarthritis symptoms by reducing inflammation or improving joint lubrication. These injections are typically administered by a healthcare provider and may be recommended for individuals who do not respond well to oral medications.
5.2.4. Disease-modifying Osteoarthritis Drugs (DMOADs)
DMOADs are a class of medications under development that aim to slow or halt the progression of osteoarthritis by targeting the underlying mechanisms of joint damage. While several DMOADs are in clinical trials, none have been approved for widespread use yet.
6. Prevention and Management Strategies
6.1. Maintaining a Healthy Weight
Maintaining a healthy weight is crucial in preventing the development or progression of osteoarthritis. Excess body weight puts additional stress on the joints, especially weight-bearing joints such as the knees and hips, increasing the risk of cartilage deterioration. A balanced diet and regular exercise can help individuals achieve and maintain a healthy weight, reducing the strain on their joints.
6.2. Regular Exercise and Physical Activity
Engaging in regular exercise and physical activity is essential for promoting joint health and reducing the risk of developing osteoarthritis. Physical activity helps to strengthen the muscles surrounding the joints, providing added support and stability. Low-impact activities such as swimming, cycling, or walking are particularly beneficial, as they promote joint mobility and cardiovascular fitness without causing excessive stress on the joints.
6.3. Proper Posture and Body Mechanics
Practicing proper posture and body mechanics can help reduce joint stress and prevent the development or progression of osteoarthritis. This includes maintaining good posture while sitting, standing, and walking, as well as using proper lifting techniques and avoiding repetitive movements that can strain the joints.
6.4. Injury Prevention
Preventing joint injuries is essential for reducing the risk of developing osteoarthritis. This can be achieved by participating in regular physical activity to maintain strong muscles and flexible joints, using protective gear during sports or high-impact activities, and avoiding movements or activities that put excessive strain on the joints.
6.5. Early Detection and Intervention
Early detection and intervention are critical in managing osteoarthritis and preventing further joint damage. Individuals experiencing joint pain or stiffness should consult a healthcare provider for a thorough evaluation and appropriate treatment recommendations. Early intervention may include lifestyle modifications, physical therapy, or medications to manage symptoms and prevent the progression of the disease.
6.6. Monitoring and Managing Other Health Conditions
Managing and monitoring other health conditions, such as diabetes, heart disease, and metabolic disorders, can help reduce the risk of developing osteoarthritis or worsening existing symptoms. Regular check-ups with a healthcare provider can help identify and address potential risk factors and ensure the appropriate management of other health conditions that may impact joint health.
6.7. Education and Support
Education and support play a significant role in the prevention and management of osteoarthritis. Individuals should be informed about the risk factors, symptoms, and treatment options for osteoarthritis, empowering them to make informed decisions about their health and well-being. Support from healthcare professionals, family members, and community resources can help individuals with osteoarthritis cope with their condition, adhere to treatment plans, and maintain a high quality of life.
7. Future Directions in Osteoarthritis Research and Treatment
7.1. Disease-Modifying Osteoarthritis Drugs (DMOADs)
One of the most promising areas of research in osteoarthritis treatment is the development of disease-modifying osteoarthritis drugs (DMOADs). These medications aim to target the underlying mechanisms of joint damage and slow or halt the progression of osteoarthritis. Several DMOADs are currently in clinical trials, and if successful, they could significantly change the way osteoarthritis is managed in the future.
7.2. Regenerative Medicine
Regenerative medicine, which focuses on repairing or replacing damaged tissue, holds great potential for the treatment of osteoarthritis. Techniques such as stem cell therapy, platelet-rich plasma (PRP) injections, and tissue engineering are being investigated as potential treatments for repairing damaged cartilage and restoring joint function. While some of these techniques have shown promise in preliminary studies, more research is needed to establish their long-term safety and efficacy.
7.3. Personalized Medicine
Personalized medicine, or the tailoring of medical treatment to the individual characteristics of each patient, is another area of interest in osteoarthritis research. By identifying specific genetic, molecular, or biochemical markers associated with osteoarthritis, researchers hope to develop targeted therapies that can effectively treat the underlying cause of the disease in each individual. This approach could lead to more precise, effective, and safer treatments for osteoarthritis patients.
7.4. Biomarkers for Early Detection
The identification of biomarkers for early detection of osteoarthritis is a significant area of research. Biomarkers are measurable substances or characteristics that can indicate the presence or progression of a disease. By identifying specific biomarkers for osteoarthritis, researchers hope to develop diagnostic tests that can detect the disease in its early stages, allowing for more effective intervention and potentially slowing or halting the progression of the disease.
7.5. Improving Non-Invasive Imaging Techniques
Advancements in non-invasive imaging techniques, such as magnetic resonance imaging (MRI), computed tomography (CT) scans, and ultrasound, could play a crucial role in the early detection and monitoring of osteoarthritis. By developing more sensitive and specific imaging techniques, researchers hope to improve the accuracy of osteoarthritis diagnosis, track the progression of the disease, and evaluate the effectiveness of various treatment options.
7.6. Lifestyle Intervention Studies
Research into the role of lifestyle factors, such as diet, exercise, and weight management, in the prevention and treatment of osteoarthritis is ongoing. Large-scale, long-term studies are needed to determine the most effective lifestyle interventions for reducing the risk of osteoarthritis, slowing its progression, and improving quality of life for those affected by the disease.
7.7. Patient Education and Self-Management
Research into the most effective methods for patient education and self-management is essential for improving the quality of life and long-term outcomes for individuals with osteoarthritis. Studies are needed to identify the best strategies for educating patients about their condition, empowering them to make informed decisions about their care, and providing them with the tools and resources they need to manage their symptoms and maintain a high quality of life.
8. Impact of Osteoarthritis on Society and Healthcare Systems
8.1. Prevalence and Economic Burden
Osteoarthritis is one of the most prevalent chronic conditions worldwide, affecting millions of individuals across different age groups. The economic burden of osteoarthritis is significant, with direct costs associated with healthcare services, medications, and surgical interventions, as well as indirect costs related to lost productivity, disability, and reduced quality of life.
8.2. Aging Population
As the global population continues to age, the prevalence of osteoarthritis is expected to rise, placing an even greater strain on healthcare systems and society as a whole. Early detection, effective treatment options, and prevention strategies are crucial to mitigate the impact of osteoarthritis on individuals and healthcare systems.
8.3. Disparities in Access to Care
Access to care for individuals with osteoarthritis can vary depending on factors such as geographical location, socioeconomic status, and insurance coverage. Disparities in access to care can result in delayed diagnosis, inadequate treatment, and poorer outcomes for those affected by the disease. Efforts to address these disparities and improve access to quality care for all individuals with osteoarthritis are essential.
8.4. Public Health and Prevention Strategies
Public health initiatives focused on raising awareness about osteoarthritis and promoting prevention strategies, such as maintaining a healthy weight, engaging in regular physical activity, and practicing proper body mechanics, can help reduce the overall prevalence and impact of the disease. These efforts, in combination with early detection and appropriate treatment, can help to mitigate the burden of osteoarthritis on society and healthcare systems.
8.5. Workforce and Caregiver Challenges
The impact of osteoarthritis extends beyond the individuals affected by the disease, as it can also place a significant burden on their caregivers and the workforce. Individuals with osteoarthritis may require assistance with daily activities or support in managing their symptoms, leading to increased demand for professional caregivers and potential strain on family members who provide care. Additionally, osteoarthritis can contribute to reduced productivity and increased absenteeism in the workplace, as individuals may struggle to perform their job duties due to pain, stiffness, or limited mobility.