Everything you need to know about the vaccines
If you want to learn about different types of vaccines and their function, join us. The practice of immunization dates back hundreds of years. Buddhist monks drank snake venom to protect themselves from snake bites, and the Chinese practiced smallpox in the 17th century. To be safe against smallpox, they injected a small amount of bovine infection through their skin.
Edward Jenner, known in the West as the founder of vaccination, in 1796, vaccinated a 13-year-old boy with the smallpox vaccine and showed others the immunization against smallpox. In 1798, the first smallpox vaccine was developed. In the 18th and 19th centuries, the systematic use of mass immunization against smallpox peaked in 1979.

Louis Pasteur’s experiments led to development of the live attenuated cholera vaccine and the inactivated anthrax vaccine (1897 and 1904, respectively). The plague vaccine was also developed in the late 19th century. Between the 1890s and 1950s, the development of antibacterial vaccines expanded, and one of the vaccines developed at that time was the bacillus vaccine (bacillus Calmet Guerrin), which is still used today.

In 1923, Alexander Glenny developed a method for inactivating Caesar’s poison using formaldehyde. In 1926, the same method was used to develop a vaccine against diarrhea. The pertussis vaccine development took longer, and a full-blown vaccine was first licensed in the United States in 1948.

Viral tissue culture methods were developed between 1950 and 1985, leading to the passive polio vaccine (leishmaniasis) and the live attenuated oral polio vaccine (sabin). Widespread immunization against polio has eradicated the disease from many countries around the world. At present, attenuated strains of measles, mumps, and rubella were used to produce the vaccine.
Despite the outstanding achievements of immunization programs, some groups have always resisted vaccination. In the late 1970s and 1980s, an increase in vaccine-related lawsuits reduced vaccine production profitability and the number of vaccine companies.
The last two decades have been applying molecular genetics and the increase of knowledge in immunology, microbiology, and genomics used in the science of vaccine production. Recent advances include developing recombinant hepatitis B vaccines, the pertussis non-cellular vaccine (which contains only compounds instead of whole cells and is much less likely to cause adverse reactions), and new techniques for producing seasonal influenza vaccines.
Molecular genetics has paved the way for vaccine science. Significant advances in this area include the development of new drug delivery systems (such as DNA vaccines, viral vectors, herbal vaccines, and topical formulations), new adjuvants, the development of effective tuberculosis vaccines, and vaccines against cytomegalovirus (CV), herpesvirus (CV). Respiratory syncytial virus (RSV), staphylococcus, streptococcus, pandemic influenza, Shigella, HIV, and schistosomiasis. Therapeutic vaccines may soon be available for allergies, autoimmune diseases, and addiction. (Coronavirus Vaccine And 10 Things You Need To Know About)
Safety system
The immune system is a network of cells, tissues, and organs that work together to defend the body against harmful objects. When bacteria, viruses, and other objects enter the body, they multiply and attack the body. This invasion is called an infection, and the infection causes the disease. The immune system protects the body against disease by fighting off invasive objects.
The immune system is constantly patrolling the body. When he encounters an attacking crime, he attacks it. This is called the immune response. The immune system first warns that an infection has occurred in a part of the body. Subsequently, antibodies are produced to fight the infection. This process may take several days. Antibodies attack objects and kill them. The immune system then remembers the crime. If the mass strikes the body again, the body detects it and quickly sends specific antibodies; Therefore, the person will not get sick. This protection against a specific disease is called immunity. In many cases, the safety described above will last a lifetime.
How do vaccines work?

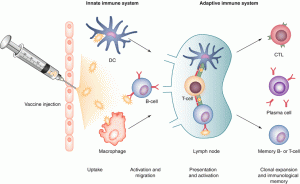
Vaccines help you get immune to the disease without getting sick. Vaccines are made from the same objects (or parts of them) that cause disease. But the objects in the vaccines are killed, or they are so weak that they cannot make a person sick. Vaccines containing these killed or weakened bodies are usually injected into the body. In this condition, the immune system reacts to the disease itself by producing antibodies to the vaccine. These antibodies kill the vaccine objects just like they kill pathogens, which is a training exercise. They remain in the bloodstream and provide immunity. If you are exposed to a real disease, they will protect you.
Vaccine safety

Vaccines are safe and effective. Because millions of healthy people, including children, receive these vaccines to prevent serious illness, they must have very high safety standards. Before a vaccine is recommended, it is tested in several laboratories. This process can take years. The Food and Drug Administration uses the information from these tests to decide whether vaccines should be tested on humans. During a clinical trial, the vaccine is tested on people who have volunteered to receive the vaccine. Clinical trials will begin with 20 to 100 participants but will eventually involve thousands of volunteers. These experiments will take several years and will answer important questions such as the following:
- Is the vaccine safe?
- What is the best dose of the vaccine?
- How does the immune system react to the vaccine?
During this process, the Food and Drug Administration works closely with the vaccine manufacturer to evaluate its safety and efficacy. All vaccine concerns must be addressed before the FDA can authorize the use of a vaccine. Once a vaccine is approved, trials continue. The company that makes those vaccines tests each group of vaccines for each of the following:
Strength: Is the effect of the vaccine as expected?
Purity: Are the components used in the vaccine production process removed from the final product?
Sterility: Does the vaccine contain no foreign matter?
Vaccines are also monitored after being recommended to the public: Once a vaccine has been licensed and recommended for use, various medical organizations continue to monitor their safety.
Side effects of vaccines
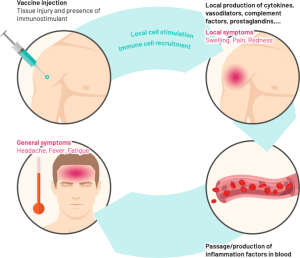
Most people have no vaccine-related side effects. Most common side effects, such as pain and discomfort when injecting, are usually mild and go away quickly. The most common side effects after vaccination include the following:
- Pain, swelling, or redness at the injection site
- Mild fever
- feeling exhausted
- Headache
- The feeling of muscle aches or joint pain
The most common side effects are signs that the body has begun to work on the immune system.
Severe side effects of vaccination
Severe side effects from vaccines are infrequent. For example, if one million doses of a vaccine are given, only 1-2 people may have an allergic reaction. Keep in mind that vaccination is much safer than getting the disease.
Some people think that if they do not get the vaccine, they can prevent the disease by consuming healthy water and observing hygiene, but this is not true. Safe water and personal and public hygiene can reduce the spread of some germs, but we do not entirely get rid of them. Some diseases, especially respiratory diseases, are spread through the air (such as measles) and are very difficult to prevent. As long as the disease is present in the environment, people will get sick.
Vaccines protect the community.
When people in a community are vaccinated, they are protecting their community in addition to themselves. This concept is called “community safety” or “herd safety.”
Crimes can spread quickly in a community and make many people sick. An epidemic will occur if the number of sick people increases enough. But when enough people are vaccinated against a disease, the crimes cannot be easily transmitted from person to person, and the disease is less likely to spread in the community. In this case, even people who have not been vaccinated will have some protection against the disease. In such cases, if a person becomes ill, the condition is less likely to become epidemic because it is more difficult to spread the disease. Eventually, the disease becomes scarce and sometimes completely eradicated from that society.
The safety of the community protects all members of that community. But in the meantime, certain groups of people, such as those who cannot be vaccinated because of certain diseases (for example, people with severe allergies and those with weakened immune systems, such as those with cancer, HIV and AIDS, and type 1 diabetes), are at a disadvantage. They will win more. Community safety is also essential for a tiny group of people who do not show a robust immune response to the vaccine.
Although many vaccine-preventable diseases may not be found in a country, it should be borne in mind that these diseases still exist in some countries. Accordingly, an epidemic will occur if foreign travelers bring the disease with them to a disease-free area. If we stop vaccinating, we will not be protected against these diseases. Community safety can only protect us if a sufficient number of people in the community are vaccinated. If you plan to travel abroad, you may need to get vaccinated to stay healthy. Depending on where you want to travel, you may contract a rare disease or illness in your country. The type of vaccine you will need before you travel depends on the following factors:
- Which country are you going to travel to? Some countries require approval for vaccinations against certain diseases, such as yellow fever or polio.
- Health status: If you are pregnant or have progressive disease or a weakened immune system, you may need other vaccines.
- Vaccines you have already received: You need to be aware of your vaccinations. Some diseases that are rare in your country may be more common in other countries.
It is essential to get the vaccine at least 4-6 weeks before the trip. This will give the vaccine a chance to get started. Also, because some vaccines are given more than once, this time interval allows you to get the full vaccine you need.
Types of vaccines
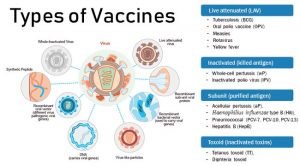
Scientists use different approaches to construction. These choices are usually made based on necessary information about the germ, such as how the germ infects the cells and how the immune system reacts to it, and practical considerations such as the region of the world where the vaccine will be used. The following are some of the options that scientists may pursue when designing a vaccine:
- Weakened live vaccines
- Inactivated vaccines
- Subunit vaccines
- Toxoid
- DNA vaccines
- Recombinant vector
Weakened live vaccines
Attenuated live vaccines contain a copy of the live germ attenuated in the laboratory and therefore do not cause disease. Because the attenuated live vaccine is very similar to a natural infection, these vaccines are a good teacher for the immune system: they elicit a robust antibody and cellular response. With just one or two injections, they provide permanent immunity to the disease.
Of course, this type also has drawbacks. The nature of living organisms is that they are altered or mutated, and organisms used in living vaccines are no exception.
It is improbable that an attenuated germ in the vaccine could become harmful and cause disease. These vaccines are also unsuitable for some people, such as people with weakened immune systems (for example, people with HIV or those undergoing chemotherapy). Another limitation is that attenuated live vaccines must be stored at a low temperature. This vaccine will not be a good option if the vaccine needs to be taken to remote areas or used in areas where there is no refrigerator.
Weakened live vaccines are relatively easy to make. Viruses are simple microbes that contain a small number of genes and can be easily controlled by scientists. These viruses are often attenuated by breeding generations of them in cells that do not reproduce well. This unfavorable environment fights viruses: as they adapt to their new environment, they become weaker than their natural host, humans.
It is challenging to produce attenuated live vaccines from bacteria. Bacteria have thousands of genes and are therefore much harder to control; However, recombinant DNA technology can delete critical genes in a bacterium. This approach has been used to produce a vaccine against the cholera-causing bacterium (Vibrio cholera).
Some essential types of attenuated live vaccines are those made against the following diseases:
- Measles, rubella, and mumps (MMR combination vaccine)
- Rotavirus
- Foolish
- Waterfowl
- Yellow fever
Inactivated vaccines
Scientists make inactivated vaccines by killing disease-causing microbes using chemicals, heat, or radiation. Such vaccines are more stable and safer than live vaccines. Killed germs cannot mutate and return to their pathogenic state. Refrigerators are usually not needed to store these vaccines and can be easily transported to different areas and suitable for developing countries. Most inactivated vaccines elicit a weaker immune response than live vaccines. Because of this, repeated vaccinations may be needed to maintain the effectiveness of the vaccine. This is a problem in areas where people do not have regular access to health care and cannot get vaccines at the right time. Some of these vaccines include:
- Hepatitis A (Hepatitis: Types, Symptoms, Treatment And Prevention)
- Influenza (injection)
- Polio (injectable)
- Rabies
Subunit, recombinant, polysaccharide, and conjugate vaccines
Certain parts of the microbe (such as protein, sugar, or capsid) are used in subunit recombinant, polysaccharide, and conjugate vaccines. Because only a fraction of the germs is used in these vaccines, the result is a robust immune response to the vaccine’s essential components. This type of vaccine can be given to anyone, including weakened immune systems and chronic health problems. One of these vaccines’ limitations is that they may need to be vaccinated several times to obtain immunity to the pathogen.
Toxoid vaccines
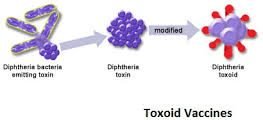
The toxoid vaccine may be effective against bacteria that secrete toxins or harmful chemicals. These vaccines are used when the leading cause of the disease is a bacterial toxin. Scientists have found that the toxin can be inactivated using formalin (formaldehyde and sterile water). Such toxins, which have already lost their toxicity, are called toxoids and are safe for vaccines.
When the immune system receives a harmless toxoid vaccine, it learns how to react to a natural toxin. The immune system will produce antibodies that inhibit that toxin. Diphtheria and tetanus vaccines are examples of toxoid vaccines.
Subunit vaccines
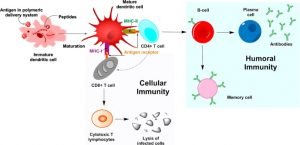
In subunit vaccines, only the antigens that stimulate the immune system are used instead of the whole germ. In some cases, these vaccines use epitopes (particular portions of the antigen that antibodies or T cells detect and attach to). Because subunit vaccines contain only the essential antigens and not other molecules that make up the germs, adverse reactions to this type of vaccine are less likely. Subunit vaccines can contain one to 20 or even more antigens. Of course, identifying which antigens stimulate the immune system best is a time-consuming and challenging process. Once scientists have done this part of the job, they can produce subunit vaccines in one of two ways:
- Cultivation of microbes in the laboratory environment, use of select chemicals to kill them, and collection of essential parts
- Construction of microbial antigen molecules using recombinant DNA technology. Vaccines based on this method are called recombinant subunit vaccines.
Injectable flu vaccines are an example of a subunit vaccine because they are made from flu viruses. A recombinant subunit vaccine has also been developed for the hepatitis B virus. The scientists inserted genes encoding important antigens (virus genes) into baker’s yeast, then collected and purified the antigens expressed in the yeast and used them to make a vaccine. Research is also underway to develop a recombinant hepatitis C virus vaccine.
DNA vaccines
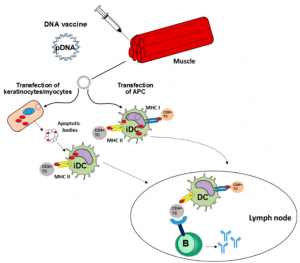
Scientists can design a DNA vaccine against a microbe by analyzing its genes. Most of these vaccines, which are still in the testing phase, have yielded promising results, and several samples are currently being tested in humans. DNA vaccines take immunization to a new level of technology. These vaccines work directly with the genetic material of the germ. DNA vaccines use genes that encode essential antigens.
Researchers have found that when the genes that make virus antigens enter the body, some cells pick up that DNA and use that genetic information to produce the corresponding antigens. In other words, the body’s cells become factories that make vaccines and make the antigens needed to stimulate the immune system.
A DNA vaccine elicits a strong antibody response to free-floating antigens secreted by cells and evoking a robust cellular response to antigens present on the cell surface. DNA vaccines do not cause disease because they do not contain germs and only have several genes. Also, designing and manufacturing DNA vaccines is relatively easy and inexpensive.
Vaccines known as naked DNA vaccines contain a type of DNA that enters the body directly. These vaccines can be given into the body using a single needle or a needleless device that uses gas pressure to throw microscopic gold particles coated with DNA into cells (gene gun: Figure below).
Sometimes DNA combines with molecules that facilitate its absorption into the cell. Examples of naked DNA vaccines are being tested for protection against the flu and herpes.
Recombinant vector vaccines
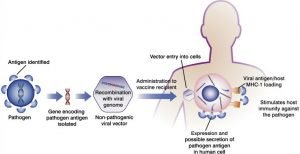
Recombinant vector vaccines are experimental vaccines similar to DNA vaccines but use an attenuated virus or bacterium to deliver microbial DNA to host cells. A vector is a virus or bacterium that is used as a carrier.
In nature, viruses attach to cells and inject their genetic material into them. Scientists are taking advantage of this process. They have figured out how to remove the spacious genome of harmless or attenuated viruses and insert parts of another microbe’s genetic material into it. Carrier viruses insert microbial DNA into the cells of the person receiving the vaccine. Recombinant vector vaccines accurately mimic a natural infection and stimulate the immune system well. Weakened bacteria can also be used as vectors. In these cases, the imported genetic material causes the bacteria to show other microbial antigens on their surface. The harmless bacterium mimics the work of a harmful microbe and elicits an immune response.
An example of a recombinant vaccine is designed to prevent diseases caused by the HPV virus; For example, the cervical cancer vaccine. In this case, the genes encoding specific proteins from the HPV virus in the vaccine are expressed to produce large amounts of that protein in the yeast. The protein that is produced is purified and then used to make a vaccine. Because the vaccine contains only one protein and not the whole virus, it cannot cause HPV infection. The immune system’s response to the recombinant protein (s) will protect the body against disease caused by the natural virus.
Herbal vaccines

Plant-based vaccines, also called herbal vaccines, are recombinant protein subunits. Ideally, selecting the plant species to produce the selected antigens should allow the appropriate vaccine’s oral delivery.
The most advanced projects of this type of human vaccine have successfully passed the first phase of clinical trials, and testing this type of vaccine in animals has yielded promising results. Producing a plant-based vaccine is done by isolating a specific antigen protein, triggering an immune response against the target virus. The gene encoding this protein is first transferred to a bacterium. Next, this bacterium will be used to infect plant cells. The plants then begin to produce a protein that will be used to make the vaccine.
The flexibility of the plant-based vaccine system with its low cost and scalability may make it possible to use this type of vaccine worldwide and in areas where other vaccines are not available. One of the most successful uses of herbal vaccines is to produce edible bananas that protect against the Norwalk virus.
Polysaccharide vaccines
The main antigens in vaccines are sugar-like substances called polysaccharides. Of course, vaccines made from pure polysaccharides are only useful in older children and adults. The pneumococcal vaccine 23 is a pneumococcal vaccine produced by 23 different bacterium strains and is an example of a polysaccharide vaccine.
Conjugated vaccines
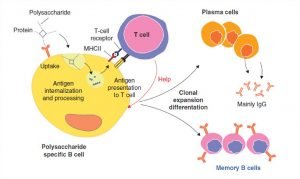
Researchers are trying to make a conjugate vaccine for it if the bacterium contains a polysaccharide outer coat. Polysaccharide coatings hide bacterial antigens; So that the immature immune system of infants and young children can not recognize them or react to them. Conjugated vaccines, which are a particular type of subunit vaccine, overcome this problem.
When making a conjugated vaccine, scientists attach antigens or toxoids from a microbe that the baby’s immune system can detect to polysaccharides. This connection helps the immature immune system react to the polysaccharide coating and fight the disease-causing bacteria. The Hib disease vaccine is a conjugate vaccine.
Advantages and disadvantages of vaccines
A vaccine is a medicine and, like any other medicine, has its advantages and disadvantages. Although vaccines are generally very convincing, no vaccine is 100% successful in preventing the disease, and no vaccine is 100% safe for all people. Most side effects of vaccines are often mild and temporary. For example, a person may feel pain at the injection site or have a mild fever. Severe reactions to vaccines are infrequent, but they can occur. The risk of injury from receiving the vaccine is much lower than contracting an infectious disease. Vaccination is an essential step for a healthy start in children.
A guide to the most commonly used vaccines
Vaccines have significantly reduced the incidence of many infectious diseases such as diphtheria, measles, and mumps. Some of these diseases have been completely eradicated from society in some parts of the world due to effective vaccination. Because of the great success of twentieth-century immunization programs, many parents today do not see many vaccine-preventable diseases and do not understand the recurrence risk. If many people decide not to vaccinate their children, some diseases that are no longer present or rare may return to the community.
Viruses and bacteria that cause vaccine-preventable diseases and death are still present in the environment and can cause illness in people who have not been vaccinated. For example, although there have been no measles in the United States since 2000, travelers from other countries have occasionally brought the virus. In December 2014, the United States experienced several outbreaks of measles. People who got measles were those who did not get the measles vaccine. Measles is one of the most contagious diseases that can cause serious problems such as pneumonia, brain swelling, and death. The prevalence of infectious diseases such as measles indicates that the best way to get rid of the disease is to get vaccinated.
The most common vaccines
DTaP vaccine
Brands: Daptacel and Infanrix
This vaccine is prepared to prevent the bacterial diseases of diphtheria, tetanus, and pertussis. Bacteria that cause diphtheria can cause throat infection and thickening of the throat, leading to breathing problems, paralysis, or heart failure. Tetanus can cause painful muscle spasms, seizures, paralysis, and death. Pertussis also has the initial symptoms of a runny nose, sneezing, and a mild cough that first looks like a common cold. The cough usually gets worse gradually, and eventually, the patient may have a severe cough that sounds like a scream. Simultaneously, as the cough occurs, the patient may vomit or become bruised due to severe shortness of breath.
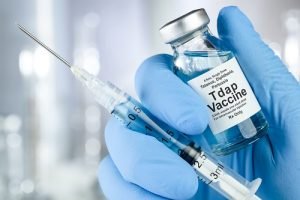
Tdap vaccine
Brands: Adacel and Boostrix
This vaccine is recommended as an immunosuppressive vaccine against bacterial infections of diphtheria, measles, and pertussis for older children. Its use is also approved for the elderly.
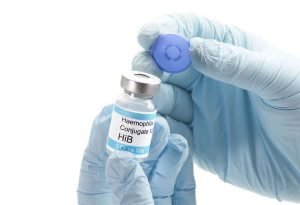
Hib vaccine
Brands: ActHIB, Hiberix, PedvaxHIB
This vaccine is designed to prevent Haemophilus flu-type b. Before the Hib vaccine became available, it was a significant cause of bacterial meningitis in many children. Meningitis is an infection of the brain and spinal cord lining that results in permanent damage to the brain and deafness. The fear of disease can also cause pneumonia, severe swelling of the throat, infection of the blood, joints, bones, epithelium of the heart, and even death.
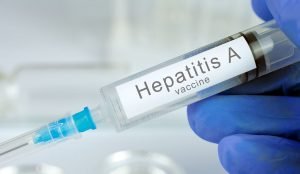
Hepatitis A vaccine
Brands: Havrix and Vaqta
This vaccine is designed to prevent illness caused by the hepatitis A virus. People infected with hepatitis A may have no symptoms or may feel mild flu or jaundice (skin or eyes), fatigue, pain, nausea, and diarrhea. Adult children with hepatitis A may have no symptoms; therefore, it is determined that the child was infected when the child-caregiver becomes ill. Hepatitis A is mostly transmitted through infected objects to the feces of a person with hepatitis A.
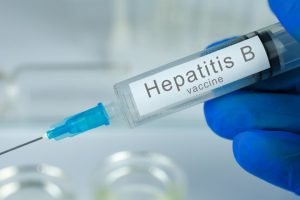
Hepatitis B vaccine
Brands: Engerix and Recombivax HB
Hepatitis B is spread when the body fluids of a person infected with the hepatitis B virus enter a healthy person’s body. Hepatitis B can cause liver inflammation, liver cancer, and death. These vaccines are approved for all ages.
Human papillomavirus vaccine
Brand Name: Gardasil 9
The HPV vaccine can be given to both sexes between the ages of 9 and 45. The vaccine prevents cervical, vaginal, and anal cancers caused by HPV types 16, 18, 31, 33, 45, 52, and 58. Overall, Gardasil 9 can prevent about 90% of these cancers.
Influenza vaccine
Brands: Afluria, Afluria Quadrivalent, Fluarix Quadrivalent, Flucelvax Quadrivalent, FluLaval Quadrivalent and Fluzone Quadrivalent
There are several vaccines available for different age groups to prevent the flu. The influenza virus is a contagious respiratory virus that can cause mild to severe illness. Older people, young children, and people with certain illnesses (such as asthma, diabetes, or heart disease) are more likely to be affected. Health problems caused by the virus can include pneumonia, ear infections, sinus infections, dehydration, or worsening conditions such as congestive heart failure, asthma, or diabetes.
Influenza strains that cause disease in humans are continually changing, so vaccination should be repeated every year to protect against the viruses that cause disease each winter. If a child has a history of Guillain-Barré syndrome, they need to talk to a specialist about getting the flu shot. This syndrome is a neurological disease that causes muscle weakness. It should also be noted that you have any allergies, including severe allergies to eggs. Due to the association between Ray Syndrome and aspirin and wild-type influenza infection, care should be taken if the child is taking aspirin or aspirin-containing therapies.
Influenza vaccine (nasal spray)
Brand: FluMist Quadrivalent
The vaccine is recommended for people 2 to 49 years of age to protect against different influenza virus strains present in the vaccine. This vaccine should also be considered if the person has a weakened immune system, asthma or recurrent mumps, or a history of Guillain-Barré syndrome. Any allergies, including severe egg allergies or aspirin use, should also be considered.
Triple measles, mumps, and rubella vaccine
Brand: M-M-R II
This vaccine is designed to prevent measles, mumps, and rubella. Measles is a respiratory disease that causes pimples, fever, cough, and runny nose. In severe cases, measles can cause ear infections, pneumonia, seizures, and brain swelling.
Mumps causes fever, headache, and loss of appetite and is a well-known symptom of swollen cheeks and jaws caused by swollen salivary glands. Rare problems such as deafness, meningitis, and painful swelling of the testicles or ovaries may also occur. Rubella, also known as German measles, can cause fever, rashes, and arthritis, especially in women. Rubella infection during pregnancy can lead to congenital disabilities.
Meningococcal Vaccines
Brands: Bexsero, Menactra, Menveo, and Trumenba
There are two different types of vaccines. One type protects four nucleated bacteria groups, called groups A, C, W-135, and Y. The FDA has approved two vaccines of this type. Another type of vaccine is a vaccine that kills a bacterium called group B. The FDA has approved these vaccines for use only in high-risk groups.
Wook’s disease is a deadly disease caused by the bacterium Neisseria meningitides. The disease causes an infection of the blood and the lining around the brain and spinal cord. Neisseria meningitides are one of the leading causes of meningitis in young children. Even with antibiotics and intensive care, between 10 and 15% of people who develop warts die from the infection.
10 to 20 percent of people also suffer from brain damage or loss of limbs or hearing. Bexsero and Trumenba are designed to prevent disease caused by serotype B of the bacterium Neisseria meningitides. Menactra and Menveo prevent meningococcal disease caused by serotypes A, C, Y, and W-135.
Pneumococcal conjugate vaccine (PCV13)
Brand: Prevnar 13
This vaccine is used to prevent invasive disease caused by 13 different types of Streptococcus pneumonia. In infants and children six weeks to 5 years of age, this vaccine is approved to prevent ear infections caused by seven different bacterium types. Streptococcus pneumonia can cause infections of the blood, middle ear, and lining of the brain and spinal cord and pneumonia. (Symptoms Of Pneumonia, Causes And Treatment Methods)
Polio vaccine
Brand: Paul
This vaccine is designed to prevent polio in infants. Polio is a disease that can cause paralysis or death. If your child is allergic to the antibiotics neomycin, streptomycin, or polymyxin B, it is essential to talk to a specialist.

Rotavirus vaccine
Brands: Rotarix and RotaTeq
The vaccine is designed to prevent gastroenteritis caused by rotavirus infection in infants. Rotavirus is the leading cause of severe diarrhea and dehydration in infants worldwide. If the child is vaccinated with a weakened immune system, blood disorders, cancer, gastrointestinal problems, a history of gastric or intestinal surgery, the specialist should be notified.
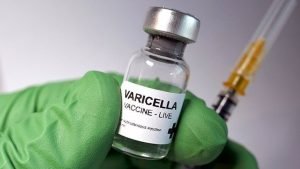
Varicella virus vaccine (chickenpox)
Brand: Varivax
Chickenpox usually causes blistering skin rashes, headaches, and fever. It can be severe in infants, adolescents, and adults, and people with weakened immune systems and causes rare problems such as skin infections, skin ulcers, pneumonia, brain swelling, Reye’s syndrome, and death.
Vaccine components
The vaccine consists of several components that are added to the safety or efficacy of the vaccine. For example, vaccine components may:
- Contribute to the safety and durability of the vaccine
- Used in vaccine production stages
- Provide immunity
Vaccine components present in the vaccine to induce an immune response:
The antigen is a minimal amount of weakened or killed germs that cause disease. Antigens help the immune system learn how to respond faster and more effectively to infections. The flu virus is an example of an antigen.
Excipients: These substances present in some vaccines are substances that boost the immune response. Aluminum is an example of auxiliary material.
Components contribute to vaccines’ safety and durability: Some vaccine components help maintain their function, and no external factors grow. Preservatives such as thimerosal protect vaccines against foreign bacteria or fungi. Preservatives are now commonly used in vaccine vials that contain more than one dose. This is because every time a vial dose is consumed, it is possible for harmful microbes to enter it. Most vaccines are available in single doses and do not use a preservative.
Some people think that the thimerosal vaccine can cause mercury poisoning, but this is not the case. Thimerosal has a different form of mercury (ethyl mercury), which does not cause poisoning, unlike methylmercury. The use of ethyl mercury in vaccines is safe because it is unlikely to accumulate in the body and is used in tiny amounts. However, most vaccines do not contain this substance at all.
Stabilizers such as sugar or gelatin help keep the active ingredients in the vaccine active during the production, storage, and relocation stages. Stabilizers prevent the active components of the vaccine from being altered by factors such as temperature. Stimulants added to vaccines include sugars such as sucrose and lactose, amino acids such as glycine or glutamic acid salts, and proteins such as human serum albumin or gelatin. Sugars, amino acids, and proteins are not limited to vaccines and are present in the daily diet, and are among the substances found naturally in the body.
Substances used during vaccine production.
Some materials are only necessary during the production process, and their final product presence is unnecessary. These substances are removed after the vaccine is produced, so only a small number remains in the final product. Tiny amounts of these components that remain in the final product are not harmful. Examples of substances used in some vaccines are:
- Cell culture materials such as eggs that help the growth of antigens in the vaccine
- Antimicrobial (inactivating) components, such as formaldehyde weaken or kill viruses, bacteria, or toxins in a vaccine.
- Antibiotics such as neomycin to prevent the growth of foreign microbes in the vaccine
Some vaccine-related concerns
Certain antibiotics may be used to prevent bacterial contamination during the production of some vaccines. As a result, small amounts of antibiotics may be present in some vaccines. There are concerns about antibiotics in vaccines because some antibiotics can cause severe allergic reactions in susceptible individuals. However, antibiotics that are more likely to cause an allergic reaction (such as penicillin, cephalosporins, and sulfa drugs) are not used in vaccines. Examples of antibiotics used during vaccine production include neomycin, polymyxin B, streptomycin, and gentamicin. Some of the antibiotics used in the production of vaccines are present in tiny amounts in the final product. For example, antibiotics are used in some methods of producing inactivated influenza vaccines. These antibiotics reduce bacteria’s growth in the vaccine’s eggs because they are not sterile. The antibiotics used reach tiny amounts during the purification process, and these small amounts have not been associated with severe allergic reactions.
Eggs are also used in some vaccines, and some people are allergic to eggs. Although severe reactions to these vaccines are unlikely to occur, people with severe egg allergies should discuss the matter with a specialist before receiving the vaccine and get the vaccine under the supervision of an expert who can manage severe allergic problems. Eggs are used in the production of influenza vaccines.
Another substance used in the vaccine production process is formaldehyde, a concern for people because of its possible cancer association. Formaldehyde has long been used in the production of vaccines against specific viruses and bacteria. It is used to inactivate viruses so that viruses cannot cause disease. Formaldehyde is diluted during the vaccine production process, but small amounts may be found in the final product. The amount of formaldehyde in some vaccines is less than the amount of formaldehyde naturally present in the body and does not cause concern.
Formaldehyde is produced in the human body as a natural product of the body’s natural functions to produce energy and make essential amino acids. It is also found in the environment and is used in building materials, laboratory materials, and many household products.
The body also processes formaldehyde continuously, and when formaldehyde is broken down, it does not distinguish between the formaldehyde vaccine and the formaldehyde naturally produced in the body. The amount of formaldehyde in a person’s body depends on their weight: the amount of formaldehyde in the baby’s body is lower; however, this is 50 to 70 times the total amount formaldehyde that can enter the body through the vaccine.
Excessive exposure to formaldehyde can cause cancer, but the main risk of formaldehyde is inhalation, and people who are generally exposed to the substance at work are at risk. No association has been found between cancer risk and exposure to low levels of formaldehyde in the vaccine.
Vaccines that use aluminum also contain only tiny amounts of this element. Vaccines containing aluminum have been tested for decades for safety, and studies have shown that the use of aluminum in vaccines is safe. Aluminum salts are used as an adjuvant in some vaccine formulations. An adjuvant is a substance that is added to some vaccines to boost the immune response. Aluminum hydroxide, aluminum phosphate, alum (potassium aluminum sulfate), or a combination of different salts of this type of material used in the vaccine. Example: Aluminum salts are used in DTaP vaccines, pneumococcal conjugate vaccines, and hepatitis B vaccines.
Vaccines containing aluminum excipients rarely cause severe reactions. The most common sources of exposure to aluminum are food and water.
Also read:
everything about kidneys? What are the functions of the kidneys?
Everything about the lungs; Know the function, disease, and treatment of the lungs
Anemia: all about the symptoms, causes, and treatments of anemia