early warning signs of osteoporosis
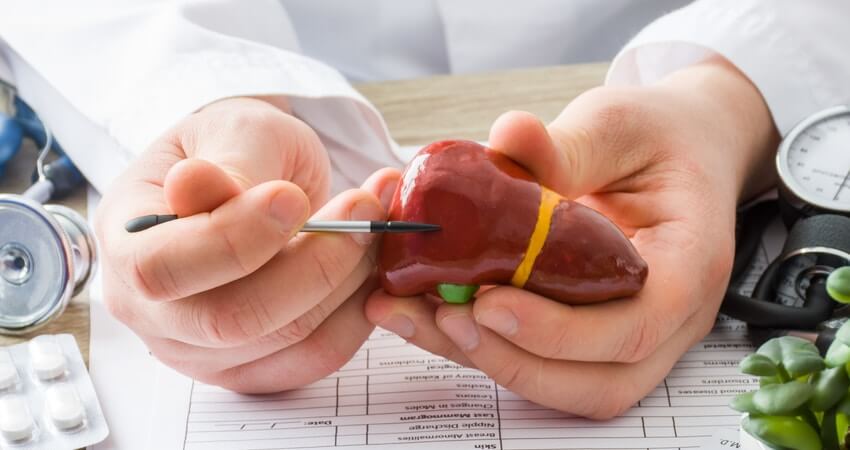
The structural and strength properties of bones are affected by osteoporosis, which increases the risk of fractures, particularly in the spine, pelvis, and wrist. Although this disease is more prevalent in postmenopausal women, smoking and a poor diet can also raise the risk. Typically, osteoporosis has no apparent symptoms, but weakened spinal bones can cause bending and bone pain. DEXA, an X-ray scan, is used to diagnose this condition, and treatment includes medications to prevent or decrease bone density loss, as well as dietary adjustments such as consuming more calcium, magnesium, and vitamin D.
Osteoporosis Outbreak Status
Osteoporosis causes over 9.8 million fractures globally each year. Approximately 200 million women worldwide have osteoporosis, and it is predicted that by 2050, the rate of pelvic fractures caused by osteoporosis will increase by 310% in men and 240% in women compared to 1990. In 2010, 50,000 pelvic fractures were reported worldwide, and this number is anticipated to reach 62,000 by 2020. Osteoporosis and osteopenia are prevalent issues among individuals over the age of 30 worldwide. The increasing trend of this disease in recent years highlights a significant global health concern. However, due to the lack of coordination among different studies’ findings, it is impossible to accurately estimate the prevalence of this disease in high populations. Osteopenia is a condition in which bones are weaker than usual, but not yet as fragile as osteoporosis.
What is Osteoporosis?
Osteoporosis occurs when bone density decreases, and the body produces less bone than it previously did. This issue can affect both men and women, but postmenopausal women are more likely to develop it due to a sudden decrease in estrogen, a hormone that naturally protects against osteoporosis. As the bones become weaker, they are more prone to breaking due to a fall or even a minor blow.
The term osteoporosis means porous bone, as bones become weaker and more vulnerable to fractures, particularly in the pelvis, spine, and wrists. Bone tissue is constantly being replaced, with new bones replacing old, damaged ones, which helps maintain bone structure and density. Bone density peaks at around 25 to 30 years of age, after which the bones begin to weaken. As we age, bone breakdown outpaces bone formation, and if this process is excessive, the result is osteoporosis.
Osteoporosis often develops slowly and may not present any physical symptoms until a person experiences a fracture from a minor fall, sneeze, or cough. Spinal fractures can cause changes in posture and curvature of the spine.
There are several risk factors for osteoporosis, some of which are modifiable while others are not:
- Age: The risk of osteoporosis increases after age 35, particularly after menopause.
- Decreased sex hormones: A decline in estrogen levels can make it harder for bones to proliferate. Maintaining hormonal balance is crucial for building and maintaining bone strength.
- Ethnicity: Caucasians and Asians are at higher risk for osteoporosis.
- Bone structure: Long or narrow bones have a higher risk.
- History of fracture: Those who have experienced fractures before are more likely to develop osteoporosis, especially after age 50.
- Eating disorders: Anorexia nervosa or bulimia nervosa can increase the risk of osteoporosis.
- Excessive alcohol consumption
- Low levels of calcium, magnesium, and vitamin D due to dietary factors, absorption problems, or medication use.
- Genetic factors: A family history of fractures or osteoporosis increases the likelihood of developing the condition. Some individuals have a higher genetic predisposition to osteoporosis. Genetic predisposition is passed down from parents and determines a person’s peak bone density. However, strategies can reduce the risk or severity of the disease in those with a genetic predisposition.
Exercise and Weight-bearing Activities: Engaging in weight-bearing exercises can be effective in preventing osteoporosis by promoting bone growth through pressure stimulation.
Medications and Health Conditions: Certain medications and health conditions can cause hormonal changes and decrease bone mass, increasing the risk of osteoporosis. Health conditions that affect hormone levels include hyperthyroidism, parathyroid disorders, and Cushing’s disease. Diseases that increase the risk of osteoporosis include cancer, chronic obstructive pulmonary disease (COPD), chronic kidney disease, and autoimmune diseases such as rheumatoid arthritis. Medications that can contribute to osteoporosis include thyroid hormone, anticoagulants and blood thinners like heparin and warfarin, proton pump inhibitors (PPIs) and other antacids that affect mineral status, some antidepressants, retinoids, thiazide diuretics, thiazolidinediones (used to treat type 2 diabetes), some immunosuppressive agents like cyclosporine, and aromatase inhibitors and other treatments that suppress sex hormones. Additionally, some chemotherapeutic agents used to treat breast and prostate cancer can contribute to osteoporosis. The most common type of medication-induced osteoporosis is glucocorticoid-induced osteoporosis.
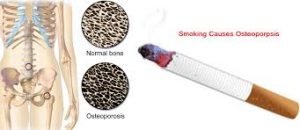
The well-known health problems caused by smoking include heart disease, lung and esophageal cancer, and chronic lung disease, with the Centers for Disease Control and Prevention reporting more than $75 billion in annual smoking-related healthcare costs in the US. For over 20 years, smoking has also been discussed as a risk factor for bone fractures and osteoporosis, with recent studies showing a direct link between tobacco use and reduced bone density. However, determining the exact effects of smoking on bone health is complex, as many smokers tend to have other risk factors like a less healthy diet, less physical activity, and more alcohol consumption. Additionally, women who smoke tend to go through menopause sooner than non-smokers, which can also contribute to osteoporosis risk. Nonetheless, most studies agree that smoking increases the risk of bone fractures, with evidence showing that the more a person smokes, the greater their risk of bone fractures in old age, and that smokers who break bones need more time to heal and may have more complications during the healing process.
Fortunately, quitting smoking can help reduce the risk of bone loss and fractures, though it may take longer for those with a long smoking history. When diagnosing osteoporosis, physicians will typically assess a patient’s family history and risk factors before requesting a bone density scan to determine the bone mineral density (BMD) using X-ray technology like DEXA (or DXA). The scan, combined with risk factor information, can indicate the possibility of osteoporotic fractures and help monitor treatment progress. Finally, it’s worth noting that a healthy person’s bone density serves as the T scale baseline in a bone density scan.

There are two types of devices used for DEXA scans:
Central Scanner: This type of scanner is located in hospitals and measures the mineral density of a patient’s pelvis and spine while they lie on a table. The scan is painless and takes around twenty minutes to complete. An X-ray generator measures the amount of calcium and other bone minerals in a specific bone to determine its mineral density.
Lateral Scanning Device: This mobile device is used to examine the bones of the wrist, heel, or fingers and is commonly available in pharmacies. However, it may not provide an accurate measurement of bone density. If the test is positive, it is necessary to see a doctor for further tests.
When interpreting the DEXA test results, two scores are used: T score and Z score. The T score compares the patient’s bone mass to the maximum bone mass of a young person, with scores above 1 being considered normal, scores between 1 to 2.5 indicating a slight decrease in bone density, and scores below -2.5 indicating osteoporosis. The Z score compares the patient’s bone mass to other people of the same age and structure, with a score of -2.5 or less indicating a risk factor for osteoporosis.
The therapeutic goals for osteoporosis include preventing its progression, maintaining proper mineral density and bone mass, reducing fractures, relieving pain, and maximizing daily functioning. Medications, such as bisphosphonates, estrogen agonists (SERMs), calcitonin, parathyroid hormone, and RANKL ligand inhibitors, can help prevent and treat osteoporosis.
Other types of estrogen and hormone therapy may also be effective in treating osteoporosis. Certain lifestyle changes can also reduce the risk of osteoporosis, such as consuming enough calcium and vitamin D. Adults aged 19 years and older should consume 1,000 milligrams of calcium daily, while women over 51 years and all adults over 71 years should consume 1,200 mg of calcium a day. Calcium-rich foods include dairy products like milk, cheese, and yogurt, as well as vegetables like broccoli and fish with soft bones, such as trout and tuna. If an individual’s calcium intake through diet is insufficient, supplementation is an option.

Vitamin D is essential for bone health as it helps the body absorb calcium. Although it can be found in dietary sources such as saltwater fish, liver, and fortified foods, most vitamin D comes from sunlight exposure. Therefore, it is recommended to have moderate exposure to sunlight. To increase bone mass for treatment, a daily intake of 600-800 units of vitamin D is required, while lower levels of 200-400 units per day can prevent osteoporosis. Many calcium supplements and multivitamins contain vitamin D.
Nutritional or drug interactions can affect calcium absorption. Certain calcium supplements are better absorbed than others, and some foods such as spinach, rhubarb, and whole grains can reduce calcium absorption by binding to calcium. Calcium can also bind to some oral drug compounds and reduce their absorption. To avoid these issues, calcium supplements should be taken one to two hours before or two to four hours after taking drugs such as sucralfate, tetracycline, ciprofloxacin, and moxifloxacin. Thiazide diuretics, like hydrochlorothiazide, can increase calcium levels and lead to poisoning.
Taking calcium or vitamin D supplements may cause side effects. Calcium can cause constipation, nausea, or vomiting, and those with kidney stones should check their calcium level in urine before increasing calcium intake. High doses of vitamin D for long periods can cause intoxication and symptoms such as weakness, headache, drowsiness, muscle aches, bone pain, and elevated liver enzymes. Those with allergies to supplements, vitamin D poisoning, or increased concentration of calcium in the blood should not take calcium or vitamin D supplements.

Treatment of osteoporosis with estrogen:
Estrogen can be taken orally in the form of pills or capsules, or applied as a skin patch. It is commonly used as part of postmenopausal hormone replacement therapy (HRT) or alone after ovarian removal. For women with uterine fibroids, progesterone may also be prescribed along with estrogen to lower the risk of uterine cancer. However, women with a history of breast cancer or family members with breast cancer should avoid taking estrogen. Other options for preventing and treating osteoporosis are being developed to reduce the risks associated with hormone use. The use of HRT for postmenopausal women is controversial due to the increased risk of cancer, stroke, and heart attack.
How does estrogen work? It helps to slow down bone loss and prevent osteoporosis in women after menopause.
People with the following conditions should not use estrogen:
Estrogen sensitivity, estrogen-related cancers such as breast cancer during pregnancy, blood clotting disorders, and unusual vaginal bleeding that has not been examined by a doctor.
General guidelines for using estrogen:
The amount of estrogen used, with or without progesterone, should be effective in achieving treatment goals. Oral tablets are usually taken daily, and for those who also require progesterone, it may be prescribed as a combination or at different times of the month. Skin patches are applied to the abdomen, pelvis, or buttocks, and the timing of changing the patches depends on the type of patch used. Some patches need to be changed weekly (e.g., Klimara), and some are changed twice a week (e.g., Vivelle).
Side effects of estrogen therapy:
Estrogen may reduce the effectiveness of anticoagulants such as warfarin. According to research conducted by the WHI Institute, postmenopausal women aged 50 to 79 who received estrogen and progesterone therapy for five years had an increased risk of heart attack, stroke, breast cancer, pulmonary embolism (blood clots in the lungs), and deep vein thrombosis (blood clots in the legs). Estrogen may cause breast tenderness, weight gain, fluid retention, gallbladder disease, and vaginal bleeding, along with an increased risk of breast and uterine cancer. Estrogen also increases the risk of blood clots and may cause blood clot-related issues such as stroke, heart attack, or thrombophlebitis (inflammation of the veins). If you experience any of the following side effects, consult your doctor:
Itching, hives, swelling of the face or hands, breathing difficulties, chest lumps, pressure in the upper right side of the stomach, vomiting, fever, pain, changes in vision, severe headaches, bloody cough, chest pain, or pain in the sole of the foot.

To prevent osteoporosis, lifestyle factors such as not smoking, limiting alcohol consumption, and doing regular exercises, including walking, for bone health and muscle strength are important. Flexibility and balance exercises, like yoga, can also help reduce falls and fractures. People with osteoporosis can benefit from a focus on nutrition, exercise, and fall prevention to reduce risks.
Looking towards the future, stem cell-based therapies may become a treatment option for osteoporosis. Studies have shown that growth hormone and calcium and vitamin D supplements can help reduce fracture risks in the long run. Research also suggests that a diet high in soy protein and isoflavones may protect postmenopausal women from bone loss. Scientists are investigating the genetic factors that contribute to bone formation and loss, in hopes of developing new ways to prevent osteoporosis.
Osteoporosis can cause constant pain, flexion, and an increased risk of fractures as bones weaken. Recovery can take longer as you age, making it essential to prevent falls to maintain independence.