Bipolar disorder; Everything about symptoms and cause and treatment
People with bipolar disorder experience severe mood swings that affect their thinking, behavior, and actions.
The following guide is for people with the disease, their families, and anyone who wants to understand the disease’s basis and its treatment and management. This guide is not a substitute for treatment provided by your doctor or healthcare provider but can be used as a basis for asking questions and discussing the disorder.

What is bipolar disorder?
Everyone has fluctuations in mood. Feelings of joy, sadness, and anger are normal. Bipolar disorder (or AIDS) is a medical condition in which a person experiences severe mood swings. A person’s mood may not be related to the events of their life. These fluctuations affect not only mood but also the way people think, behave, and act. Bipolar disorder is not the fault of the individual or is due to a weak or unstable personality. This disorder is a medical disorder that can be treated.
About one to two percent of adults worldwide have the disorder. The prevalence of this disorder is equal in men and women.
When does bipolar disorder start?

In most cases, the first symptoms of this disorder are diagnosed during puberty or early adulthood. However, the younger the age at which the first symptoms appear, the more unusual the symptoms. Symptoms may be confused with adolescent anxiety or rebellion, so bipolar disorder is often undiagnosed until adulthood. In some women, the disease can occur during or shortly after pregnancy. Post-pregnancy mania is present in only one in every 1,000 mothers. Postpartum depression is more common.
Clinical features of bipolar disorder
Episodes of Bipolar Disorder: This disorder is recurrent and has periods. This disorder usually consists of three stages:
- High state (high mood) is called mania
- Low mood (low mood) is called depression
- A good situation in which many people feel normal and perform well
Mania and depression may consist of pure episodes (symptoms of mania or depression only) or mixed episodes (a combination of symptoms of mania and depression at the same time). Often, mixed episodes are associated with the disease mania stage, so terms such as mania and dysphoric mania are often used to describe complex states.
Types of bipolar disorder
Some people experience manic (or mixed) depression, depression, and well-being during their illness. Such people have this type 1 disease. It is called a milder form of hypomania. People with hypomania, depression, and asymptomatic intervals with complete manic episodes have type 2 bipolar disorder. (What Is Depression? Everything About Depression, Symptoms, And Treatments)
Sequence and frequency of different states of bipolar disorder
Mania, hypomania, confusion, and depression usually do not occur in a specific order, and their frequency cannot be predicted. There is a gap of several years between each episode for many people, while others experience more frequent episodes. A person with bipolar disorder experiences an average of about ten episodes of depression and mania/hypomania or mixed states in their lifetime. As we age, the episodes of the disease often get closer together. Untreated mania often lasts two to three months. Untreated depression usually lasts between four and six months.
Rapid-cycle bipolar disorder
About 20% of people with the disorder experience four or more periods during the year
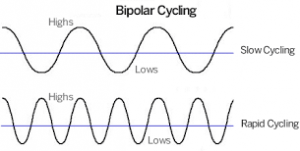
In this case, they are said to have a rapid cycle, a disorder that requires special treatment. We do not know for sure what causes the rapid cycle. Certain antidepressants may trigger it, but it is not clear how antidepressants cause a rapid cycle. Sometimes stopping taking an antidepressant may help a person return to a regular cycle pattern.
Symptoms of bipolar disorder
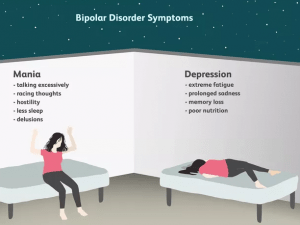
Mania
Occasionally, a person may appear abnormal, irritable, or open-minded for at least a week at a time. If these mood swings are accompanied by other symptoms (listed below), they may be in the manic phase of bipolar disorder. Not everyone who enters the stage of mania feels happy. Instead, the person may feel very irritable or very angry, upset, and aggressive. People in a manic phase do not just have mood swings. To diagnose a manic episode, they must have at least three of the following symptoms:
False self-esteem or self-aggrandizement: People feel invincible or strongly empowered. They believe that they understand how the world works or how to save it. They may feel that they have a special mission in life (God has sent them or give them special powers).
Less need for sleep: People may feel refreshed after a little sleep. Sometimes they may not sleep at all for days or weeks.
Talkative: Affected people speak very fast, very loudly, and much more than usual. They may like to say jokes or rhyming words and get angry when they are interrupted. They may change topics and not be able to communicate appropriately with others.
Jumping Thoughts: People are easily distracted and have difficulty interacting because they are easily distracted.
Increased activity: People may become more social or active than usual at school or work and look very energetic. In the early stages of mania, they may be productive, but as the symptoms worsen, they become overwhelmed with their activities and start many projects but do not finish them.
Poor Judgment: People may not be able to control or plan how they act. They may engage in unusual and risky activities (such as over-purchasing, poor business choices, and bad decisions) without realizing the harmful consequences. They may become more sexually active and less careful in choosing their sexual partner. An increase in sexual activity may lead to unwanted pregnancies, sexually transmitted diseases, guilt, and failed relationships.
Symptoms of psychosis: People may experience symptoms of psychosis such as delusions (beliefs that are not based on reality). They may have such illusions. These people often hear sounds that do not exist.

Hypomania
The symptoms of hypomania are less than the symptoms of mania. However, they can be destructive. People may feel happy and have a lot of energy, but they usually do not have serious problems. Hypomania can progress to episodes of complete mania or severe depression and therefore require treatment.
Mixed mode
Some people do not always have pure episodes of mania or depression. Instead, they may experience episodes in which symptoms of mania and depression co-occur. This is called a mixed state. For example, a person in a mixed state may think and babble. At the same time, the person may be very anxious and have suicidal thoughts. Mixed conditions are challenging to diagnose, and this condition is excruciating for the person.

Depression
Depression can take many forms, and it is often unclear where it comes from. Symptoms must persist for at least two weeks and most days. Symptoms of depression in bipolar disorder include at least five of the following:
mood: The mood in depression is significantly different from normal sadness. Many people who experience depression say that they can not feel sad, and many can not cry when depressed. The ability to cry again often means relieving depression.
Loss of interest or enjoyment in previously fun activities: When people start feeling depressed or mildly depressed, they can still enjoy things and focus on enjoyable activities. When people are severely depressed, they lose these abilities.
Weight Loss or Weight Loss: Many people lose weight when they are depressed, in part because they lose their appetite. However, many people feel more hungry and may be more inclined to eat carbohydrate-rich and fatty foods. This leads to weight gain. Also, metabolism may increase or decrease depending on the type of depression, leading to weight gain or loss.

Sleep problems: Sleep disorders are common in depression. Many people experience insomnia: they have trouble falling asleep and often wake up during the night or very early in the morning. For these people, sleep is not relaxing, and they wake up feeling tired. Other people, especially during the day, sleep too much and have so-called oversleeping.
Indifference or confusion: Many people with depression experience slowness of movement, speech, or thinking. In severe cases, people with depression may not be able to move, speak, or respond to their environment. For some people, the opposite is accurate, and they are agitated. They suffer from severe internal restlessness. They can not sit still, walk around and clasp their hands. People who feel mentally restless have anxiety as well.
Decreased energy: Completing daily tasks becomes difficult for people with depression. Because they lack energy and motivation, it takes more time to do work or home-related tasks.
Feelings of worthlessness and guilt: When depressed, people may lose confidence. They may be overwhelmed by feelings of worthlessness. Many of them can not stop thinking about the past. They are obsessed with feeling bad about others or saying the wrong things, and they feel very guilty. In severe cases, this guilt may cause delirium. In this situation, people are sure that they are guilty and should be punished for their wrongdoings.
Inability to concentrate or make decisions: These symptoms can be so bad that people cannot perform simple tasks. They may have difficulty deciding on minimal issues.

Suicidal thoughts: Depressed people often think that life has no value or better not to live. The risk of committing suicide based on these thoughts is very high, and many people commit suicide when they are depressed.
Symptoms of Psychosis: Symptoms of psychosis in depression may include misconceptions about poverty or being punished for past sins. People may think they have a deadly disease like cancer. They may also hear sounds or see things that do not exist.
Symptoms of depression
Symptoms of depression often include the following:
- Severe anxiety
- Worrying about small issues
- Complaints about physical symptoms, including pain
- Frequent visits to the doctor for various physical symptoms
Other symptoms of a bipolar episode
Some people with bipolar disorder may have movement disorders during episodes. These motor symptoms occur in 25% of patients with depression and up to 28% of patients with mixed episodes of pure mania. Movement problems, called catatonic symptoms, are variable and can include severe physical restlessness, slowness, or strange movements and postures. People sometimes can’t relax. Others move so slowly that they refuse to open their mouths to eat, drink, or talk. In most cases, people get rid of motor symptoms after specific treatments. There is a risk that people with these symptoms will be misdiagnosed because they are more likely to be associated with schizophrenia.
Comorbidity and its importance in bipolar disorder
Comorbidity disorder is a medical condition or condition that occurs with another medical condition or condition. Comorbid conditions can occur at the same time as bipolar disorder. They can start before or at the same time as bipolar disorder. Experts do not know why some disorders occur more frequently at the same time as bipolar disorder. The severity of the comorbidity may change throughout life, and its symptoms may change as bipolar disorder changes. For example, alcohol is one of the most common comorbid conditions. People with alcohol problems may overdose on alcohol or try other medications. They may also take drugs during the depression phase because they believe it helps them feel less depressed. These same people may not turn to alcohol or drugs at stages when they are mentally well.
Psychiatric conditions that often co-occur with bipolar disorder include:
- Panic disorder
- Obsessive-Compulsive Disorder
- Overeating disorder
- Drug abuse
- Attention Deficit Hyperactivity Disorder
- Borderline personality disorder
Diagnosis of comorbidity is vital in bipolar disorder. Comorbid conditions may affect the clinical picture and complicate the treatment of bipolar disorder. Also, comorbid conditions are often so severe that they also need treatment.

What causes bipolar disorder?
Various factors are involved in causing bipolar disorder, and its exact mechanism is unknown. However, there is strong evidence that biological factors, including genetics, play an essential role. This does not mean that a person must inherit genes: the genes involved may change when a person is formed. Scientists believe that a change in genes could lead to defective proteins within brain cells, leading to bipolar disorder. Researchers are studying different genes as well as proteins that may be affected by bipolar disorder.
Bipolar disorder is not caused by severe stress or family problems. However, these factors may trigger an episode of illness in a person who already has the disorder. Bipolar disorder is also not the result of a simple imbalance between neurotransmitters such as serotonin or dopamine. However, neurotransmitters may be affected during the onset of the disease.
What is the trigger for bipolar disorder episodes?
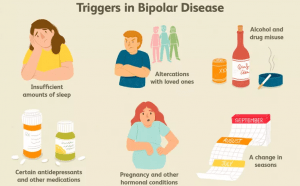
A single primer can cause not all disease episodes, but one primer can trigger many episodes. Initiators are conditions that can trigger mania or depression in a person who has already experienced an episode of illness. Feelings of extreme stress or persistent lack of sleep are examples of these types of initiators. Other primers include chemicals and antidepressants that have a “very high” effect and lead to mania. Common medications such as steroids (such as prednisolone, which is used to treat asthma, arthritis, and others) and street medications such as cocaine and amphetamines are also in this category. (Asthma Disease: Symptoms, Cause, Diagnosis, And Treatment)
Treatments for bipolar disorder
Treatment for bipolar disorder includes biological therapies (medications) and psychosocial therapies (psychotherapy and psychotherapy). Both treatments are often needed, but biological treatment is usually done first to control the symptoms.
Biological therapies: Because bipolar disorder has a vital biological component, the primary forms of treatment are biological. These include mostly medications, but other therapies such as phototherapy and electroconvulsive therapy and magnetic stimulation of the brain are also used.
Drugs used to treat bipolar disorder: Medications are the cornerstone of treating bipolar disorder. They are needed to restore and promote health and prevent the recurrence of symptoms. There are usually several medications for bipolar disorder. Finding the right medication and amount for the sick person requires constant monitoring and conversation with the doctor.
If the symptoms of bipolar disorder are not treated, they may return—most people who have not been treated experience another episode within a year or two. Medications not only treat the symptoms but also prevent the disease from coming back. People who continue to take their medications are more likely to stay in good shape.
For some people who experience a single mild episode that is not very disabling, taking medication for up to a year or two may be enough. However, for most people, long-term treatment is recommended. In many cases, treatment may last a lifetime. Bipolar disorder is potentially a chronic medical condition.
Sometimes people with bipolar disorder may feel well for a long time. When this happens, the disease may have entered a calm phase, or medications may have successfully prevented the symptoms. In any case, it is essential to continue taking medicine. If a person stops treatment, there is an 80% chance that the disease will recur within two years. Recurrence may even occur after years of stabilization.
Some people worry about drug addiction or personality change. The main treatments for bipolar disorder are mood stabilizers, antidepressants, and antipsychotics. These drugs are not addictive, and there is no evidence that they cause personality changes. However, some anxiety medications risk addiction if taken regularly for more than a few weeks.
Some medications used to treat bipolar disorder may have side effects. Many side effects are reduced over time, and others can be relieved with a doctor’s help. The doctor will monitor for side effects and the amount of medication and sometimes perform other tests. With these studies, the risk of long-term physical side effects from medications is low. The risk of living with untreated bipolar disorder is much higher.
The drugs used to treat bipolar disorder fall into two broad categories: mood stabilizers and adjuvants.
Complementary Medications: Complementary medications are medications used to treat specific symptoms such as depression, poor sleep, anxiety, and psychotic symptoms. Complementary medications include antidepressants, anxiolytics, and antipsychotics. These drugs are often used for a short time until the mood stabilizers show their full effect. However, they may also be used to combine mood stabilizers as a longer-term treatment for bipolar disorder. People with bipolar disorder often need more than one medication.

Mood stabilizers: Mood stabilizers are drugs that help reduce mood swings. These medications also help prevent episodes of mania and depression. The oldest and most well-known mood stabilizer is lithium.
Many of the drugs that were initially developed as anticonvulsants to treat epilepsy also act as mood stabilizers. These include carbamazepine, Divalproex, and lamotrigine. Gabapentin and topiramate are also anticonvulsant drugs that may also act as mood stabilizers, although they are usually prescribed in combination with other drugs.
Some people may be prescribed more than one type of mood stabilizer to take in combination. How mood stabilizers work is not fully understood, although they are thought to somehow calm or prevent the brain’s over-stimulated areas from progressing.
The side effects of mood stabilizers vary depending on the drug. For some drugs, side effects are kept to a minimum by continually monitoring the drug’s level in the blood. Some people do not experience side effects. For some, the side effects can be annoying. Side effects usually decrease as the treatment process continues. If side effects are not tolerable, you should see a doctor as soon as possible.

Lithium: Lithium is found in some mineral waters and is present in small amounts in the human body. Lithium is used to treat mania and prevent subsequent episodes of mania and depression. There is evidence that lithium protects brain cells from inflammation that occurs in people with bipolar disorder.
Common side effects of lithium include increased thirst and urination, nausea, weight gain, and mild hand tremors. Less common side effects include fatigue, vomiting and diarrhea, blurred vision, memory impairment, difficulty concentrating, skin changes (such as dry skin or acne), and minor muscle weakness. In general, these effects are mild and go away with continued treatment. However, if any of these side effects are severe, you should see your doctor. In some people, thyroid and kidney function is affected by lithium and should be monitored regularly by a physician.
Divalproex, valproic acid, or valproate: The different names of this anticonvulsant drug indicate its formulation’s different methods. Di Valproix (and its various forms) is used when people have frequent mood swings or are not affected by lithium. Common side effects of Di Valproix include drowsiness, dizziness, nausea, and blurred vision.
Carbamazepine: Carbamazepine is another anticonvulsant. It is used to treat mania and mixed conditions that do not respond to lithium or when the person is irritable or aggressive. Side effects of carbamazepine include dizziness, drowsiness, blurred vision, dizziness, muscle tremors, nausea, vomiting or mild abdominal muscle cramps, increased sensitivity to sunlight, skin allergies and skin rashes, and poor coordination. One of the rare but dangerous side effects of carbamazepine is a decreased number of red blood cells. People taking this medicine should have their blood regularly monitored for this side effect. Pain in the mouth, gums, or throat, mouth ulcers and fever, and flu-like symptoms can be signs of this effect and should be reported to a doctor immediately. If carbamazepine causes these symptoms, these effects go away when you stop taking them.
Lamotrigine: Lamotrigine may be the most effective mood stabilizer for depression in bipolar disorder, but it is not beneficial for mania. The starting dose of lamotrigine should be shallow and increase very slowly over four weeks. This method reduces the risk of severe skin rashes, which is a severe side effect of this drug. Side effects of lamotrigine include fever, dizziness, drowsiness, blurred vision, nausea, vomiting, mild abdominal cramps, headache, and skin rash.
Antidepressants: Antidepressants are first known to treat depression effectively and have recently been useful in treating anxiety disorders. Antidepressants are thought to work by affecting the concentration of neurotransmitters in the brain. The significant neurotransmitters affected by these drugs include serotonin, norepinephrine, and dopamine.
While antidepressants can be used during episodes of bipolar disorder, they should be used with caution as they can change the patient’s mood to mania and lead to a cycle of recurrent mood episodes (rapid cycles). There are several groups of antidepressants, and there are many medications in each group. The different types of antidepressants are listed in order of frequency.
Selective serotonin reuptake inhibitors (SSRIs): Fluoxetine, paroxetine, fluvoxamine, citalopram, escitalopram, and sertraline. SSRIs are usually the first choice for treating depression and anxiety problems.
Selective serotonin reuptake inhibitors and norepinephrine (SNRIs): These drugs include venlafaxine, duloxetine, and desvenlafaxine.
Norepinephrine and dopamine reuptake inhibitors (NDRIs): The drug available in this group is bupropion. When used to treat depression, it is often due to its energetic effects and is prescribed in combination with other antidepressants.
Noradrenergic and specific serotonergic antidepressants (NaSSAs): Mirtazapine, the drug in this group of antidepressants, is the most sedative antidepressant.
Rings: This older group includes amitriptyline, maprotiline, imipramine, desipramine, nortriptyline, and clomipramine. Because these drugs usually have more side effects than newer drugs, they are often not the first treatment choice.
Monoamine oxidase inhibitors (MAOIs): Monoamine oxidase inhibitors such as phenelzine and tranylcypromine were the first antidepressants. Monoamine oxidase inhibitors are useful but are often not used because people on a diet must follow a special diet. One of the newer drugs in this group is moclobemide, which can be taken without dietary restrictions, although it may not be as effective as other drugs.

Anxiety medications: Anxiety is common in bipolar disorder. Sleep disturbance also occurs frequently during an acute episode. In most cases, benzodiazepines, which are a family of mild sedatives, are prescribed. All benzodiazepines work the same way, although the intensity and duration of their effects vary. Benzodiazepines may be used for short periods without addiction. The most commonly used benzodiazepines to treat anxiety include clonazepam, alprazolam, and lorazepam.
Clonazepam is especially useful for treating excessive energy and reduced sleep due to mild mania. Benzodiazepines used to treat insomnia include lorazepam, nitrazepam, oxazepam, temazepam, triazolam, and flurazepam.
Another drug used for insomnia is zopiclone. It is similar to benzodiazepines and has similar side effects. Zopiclone may have less potential for abuse than benzodiazepines, although people may become addicted to this drug.

Antipsychotic drugs: Antipsychotic drugs are commonly used in bipolar disorder. These drugs have powerful sedative effects that help control mania and treat symptoms of psychosis such as delirium, magnification or torture, and hallucinations. Antipsychotic drugs are generally divided into first-generation drugs (regular or typical) and second-generation drugs (unusual or atypical). Second-generation medications are now prescribed for most people who have been taking antipsychotic medications for a more extended time.
First Generation Antipsychotic Drugs: These older drugs include chlorpromazine, flupentixol, fluphenazine, haloperidol, lupine, perphenazine, pimozide, trifluoperazine, thiothixene, and zuclopenthixol.
Second Generation Antipsychotic Drugs: Drugs in this class include risperidone, quetiapine, olanzapine, ziprasidone, paliperidone, aripiprazole, and clozapine. Clozapine is an exception in that it is often useful even when other drugs do not work. However, it is not the first treatment option because it requires monitoring white blood cell counts.
Newer medical treatments
Many of the newest drugs used as mood stabilizers for bipolar disorder were first developed as anticonvulsants (epilepsy therapies). These include Divalproex, carbamazepine, lamotrigine, topiramate, and gabapentin. There is variable evidence for these drugs’ efficacy, and Divalproex and lamotrigine have been studied more than any other drug.
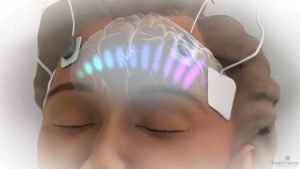
Electroshock treatment: Perhaps the most controversial and misinterpreted psychiatric treatment is electroconvulsive therapy (ECT) or electroconvulsive therapy, partly due to its portrayal in the public media.
Electroconvulsive therapy is very useful and safe in treating depression and bipolar disorder. It is sometimes used as a long-term maintenance treatment to prevent recurrence of the disease after recovery. Electroconvulsive therapy is not like what is imagined in many movies. Patients now receive muscle relaxants and general anesthesia before a light electric current is applied to one or both sides of their brains. During this procedure, there are a few noticeable movements in the patient. Treatment is usually given three times a week for a period of 3 to 4 weeks.
For more extended maintenance treatment, treatment may be given once a month for as long as the patient and physician deem appropriate. Electroconvulsive therapy is usually performed on hospitalized patients, but other patients can also receive this treatment.
Side effects of electroconvulsive therapy
Patients may experience headache or jaw pain after waking up from ECT, which is often relieved with a mild analgesic such as acetaminophen. There is usually some recent memory loss or concentration problems during treatment (for example, patients may not remember what they ate the night before treatment). Still, these symptoms improve quickly after a period of treatment and within a few weeks. Some patients report mild memory problems that persist long after treatment.
Use of electroconvulsive therapy in the treatment of the bipolar disorder

Electroconvulsive therapy is the most effective and possibly the fastest and most effective treatment for major depression. It is beneficial for people with severe mental disorders or suicidal ideation or people with psychotic or catatonic symptoms.
Some people undergo electroconvulsive therapy early in the episode due to the condition’s urgency or specific symptoms. In contrast, for others, electroconvulsive therapy may be used after other medications have failed. Electroconvulsive therapy also works well for severe mania. While electroconvulsive therapy is very useful in ending an episode of depression or mania, its benefits may only last for a few weeks to a few months after treatment. Therefore, patients usually begin or continue treatment with mood stabilizers and other medications after a period of electroconvulsive therapy. Maintenance electroconvulsive therapy may be used if medications do not prevent the disease from coming back or for patients who cannot tolerate their side effects.
Magnetic stimulation of the brain
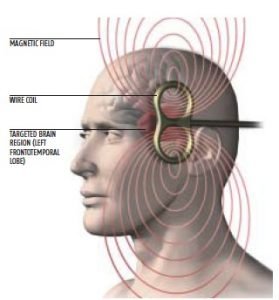
In magnetic stimulation of the brain, or more precisely, magnetic stimulation of the brain through the skull (TMS), short magnetic pulses enter the brain to stimulate nerve cells. Magnetic stimulation of the brain is being tested, but its effectiveness has not yet been confirmed. Unlike electroconvulsive therapy, this treatment is applied without the need for anesthesia or muscle relaxants.
Complementary or alternative therapies
Some people with bipolar disorder seek out unusual treatments that are often used to adjunct to complementary treatments rather than as alternatives. Examples of complementary therapies include herbal medicine, acupuncture, homeopathy, physiotherapy, meditation, yoga, and Ayurveda. Several dietary supplements and vitamins are also available.
Many of these treatments have not yet been thoroughly tested. St. John’s wort has been shown to have antidepressant effects for mild to moderate monopolar depression (mania-free depression). However, in people with bipolar disorder, it is likely to cause a change from depression to mania. St. John’s wort may also interact with several common medications. If you are interested in herbal medicines, you need to talk to your doctor.
Omega-3 fatty acids are anti-inflammatory, and omega-3 rich diets are associated with lower rates of depression. There is evidence that omega-3 fatty acids may be useful in treating bipolar depression.
Physical activity or exercise also has antidepressant effects. Regular physical activity (even just 30 minutes of walking during the day) has substantial physical and mental health effects. Exercise also increases the size of the hippocampus. The hippocampus is the part of the brain that is involved in memory.
Psychosocial therapies

Psychosocial therapies include psychotherapy, psychotherapy, support groups, and rehabilitation.
Psychoeducation: Psychological education is how people become aware of bipolar disorder and talk about their feelings and cope with the disorder. For example, many sufferers may experience feelings of fear or denial. Talking about these feelings often helps people cope with them and better adhere to their proper treatment plans.
Psychological training can be done in groups or individual consultation with a doctor, social worker, or other mental health service provider. When psychological training is provided as a group, it is usually time-limited (8 to 12 sessions). Each session focuses on a different aspect of bipolar disorder management (e.g., signs and symptoms of bipolar disorder, stress management, and problem-solving). Psychological education also helps family members understand the patient’s condition.
Although public education has increased public awareness in recent years, many people do not understand mental illness and feel uncomfortable discussing it. People with bipolar disorder must have a safe place to discuss the issue with their families and decide what information they want to share with people outside the family.
Psychotherapy: Psychotherapy is a general term used to describe a form of treatment based on a therapist’s conversation. The goal is to discuss and express emotions to help reduce anxiety. Also, he develops more useful attitudes, behaviors, and habits and adopts more constructive and adaptive coping methods.
Successful psychotherapy relies on a supportive and comfortable relationship with a trusted therapist. There are several models of psychotherapy that are generally classified into two groups: short-term and long-term. Short-term therapies are structured and focus on current issues rather than childhood issues. On average, treatment takes about 10 to 20 sessions. In short-term therapies, the therapist plays an active role in guiding the discussion. Long-term treatment is less structured and can last a year or more. The person being treated has the opportunity to talk about various concerns related to past and present issues. In this model, the therapist has a less guiding role.
Psychotherapy is a very effective treatment. However, in bipolar disorder, this method can be used as adjunctive therapy and is not a substitute for medication. Every patient should receive supportive treatment about medication management and deal with the various problems that a person with bipolar disorder may face. Practical suggestions and emotional support are the main features of supportive care.
Cognitive-behavioral therapy: Cognitive-behavioral therapy (CBT) is an example of short-term structured psychotherapy that has worked well for many other disorders. This approach is based on the idea that deep beliefs or thoughts affect our view of ourselves and the world and profoundly affect our mood and behavior. For example, if we are depressed and think that no treatment will help us, we may not seek treatment, and thus, our condition will worsen. Cognitive therapy seeks to identify and change these thoughts to improve mood and function.
Anxiety is common in bipolar disorder, and cognitive-behavioral therapy may be beneficial for more severe anxiety problems such as panic attacks. It may be necessary in some cases because antidepressants, which are sometimes used to treat anxiety disorders, can provoke episodes of mania.
Hospitalization

During severe episodes of depression or mania, some people with bipolar disorder may need to be hospitalized. Hospitalization is necessary if the disease is out of control and exposes the person to severe consequences (such as aggressive behavior, risk-taking, lack of care for basic needs, or suicidal tendencies).
Bipolar disorder is a medical disorder that can be treated. Medications are the cornerstone of treating bipolar disorder and, along with psychosocial therapies, are needed to restore and promote health and prevent recurrence of symptoms. If the symptoms of bipolar disorder are not treated, they may return.


