How do you catch pneumonia at home
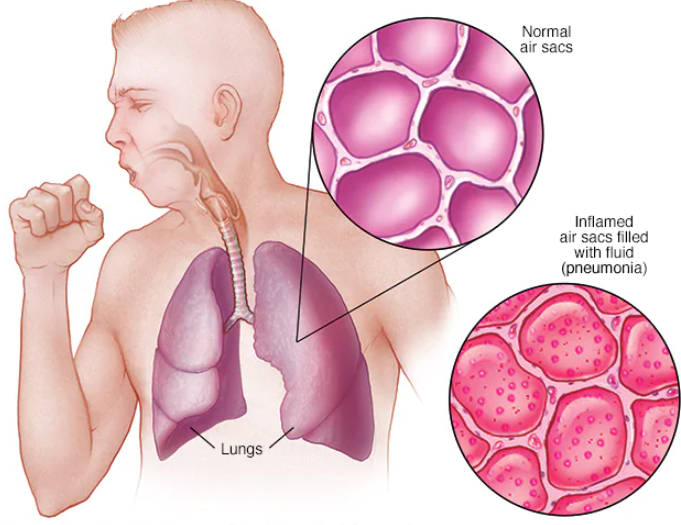
Pneumonia is a serious lung infection that can have severe consequences if not properly treated. It affects the air sacs in one or both lungs, which may fill with fluid or pus, leading to symptoms such as cough, fever, chills, and difficulty breathing. While pneumonia can be contracted in various settings, including hospitals and other healthcare facilities, it is also possible to catch pneumonia at home. Understanding how pneumonia spreads and the factors that can increase the risk of contracting it at home is crucial for prevention and management.
Causes and Types of Pneumonia
Pneumonia can be caused by various pathogens, including bacteria, viruses, fungi, and mycoplasmas. The most common types of pneumonia based on the causative agents include:
- Bacterial Pneumonia: This is often caused by the bacterium Streptococcus pneumoniae, but other bacteria like Haemophilus influenzae and Legionella pneumophila can also be responsible. Bacterial pneumonia typically occurs when the body’s immune system is weakened or compromised.
- Viral Pneumonia: Viruses such as influenza, respiratory syncytial virus (RSV), and the coronavirus (COVID-19) can cause viral pneumonia. Viral infections can be more contagious and spread easily within households.
- Fungal Pneumonia: This type of pneumonia is less common and usually affects people with weakened immune systems. Fungi like Histoplasma, Coccidioides, and Cryptococcus can cause fungal pneumonia.
- Mycoplasma Pneumonia: Mycoplasma pneumoniae is a less common cause but can still lead to a milder form of pneumonia often referred to as “walking pneumonia.”
Risk Factors for Catching Pneumonia at Home
Several factors can increase the risk of catching pneumonia at home:
- Age: Infants, young children, and the elderly are more susceptible to pneumonia because of their weaker immune systems.
- Chronic Health Conditions: Individuals with chronic illnesses such as asthma, chronic obstructive pulmonary disease (COPD), diabetes, or heart disease have a higher risk of developing pneumonia.
- Weakened Immune System: Conditions like HIV/AIDS, cancer treatments, or the use of immunosuppressive drugs can compromise the immune system, making it easier for infections to take hold.
- Recent Respiratory Infections: A recent bout of influenza or a cold can weaken the respiratory system and make it more susceptible to pneumonia.
- Smoking and Substance Abuse: Smoking damages the lungs and reduces their ability to fight off infections. Similarly, excessive alcohol consumption can impair the immune system and increase the risk of aspiration pneumonia.
- Environmental Factors: Poor indoor air quality, such as exposure to pollutants, mold, or secondhand smoke, can irritate the lungs and make them more vulnerable to infections.
How Pneumonia Spreads at Home
Pneumonia-causing pathogens can spread in several ways:
- Person-to-Person Transmission: Bacterial and viral pneumonia can spread through droplets when an infected person coughs or sneezes. Close contact with an infected person, such as sharing utensils, touching contaminated surfaces, or direct physical contact, can facilitate the spread of the infection.
- Airborne Transmission: Some viruses, including those that cause pneumonia, can be airborne and inhaled by others in close proximity. Poor ventilation and crowded living conditions can increase the risk of airborne transmission.
- Aspiration: Aspiration pneumonia occurs when food, liquid, or vomit is inhaled into the lungs instead of being swallowed into the esophagus. This can happen if a person has difficulty swallowing, often due to neurological conditions or excessive alcohol consumption.
- Environmental Contaminants: Fungal pneumonia can be contracted by inhaling spores from contaminated soil or bird droppings, which can sometimes be present in home environments, particularly in areas with poor maintenance or hygiene.
Prevention Strategies
Preventing pneumonia at home involves a combination of personal hygiene, environmental management, and medical interventions:
- Vaccinations: Immunizations are crucial in preventing certain types of pneumonia. The pneumococcal vaccine can protect against bacterial pneumonia caused by Streptococcus pneumoniae, while the influenza vaccine helps prevent flu-related pneumonia. The COVID-19 vaccine also reduces the risk of pneumonia caused by the coronavirus.
- Good Hygiene Practices: Regular hand washing with soap and water, using hand sanitizers, and covering the mouth and nose when coughing or sneezing can reduce the spread of infectious agents. Avoiding close contact with sick individuals and disinfecting commonly touched surfaces can also help.
- Healthy Lifestyle: Maintaining a healthy lifestyle by eating a balanced diet, staying hydrated, exercising regularly, and getting adequate sleep can strengthen the immune system. Avoiding smoking and excessive alcohol consumption is also crucial.
- Proper Home Environment: Ensuring good ventilation in the home, reducing exposure to indoor pollutants, and using air purifiers can improve air quality. Regular cleaning and maintenance can prevent the buildup of mold and other contaminants.
- Managing Chronic Conditions: Individuals with chronic health conditions should work closely with their healthcare providers to manage their conditions effectively. Regular check-ups, medication adherence, and following medical advice can help reduce the risk of infections.
Recognizing Symptoms and Seeking Treatment
Early recognition of pneumonia symptoms and seeking prompt medical attention is vital for effective treatment and recovery. Common symptoms of pneumonia include:
- Persistent cough, which may produce phlegm or mucus
- Fever, chills, and sweating
- Shortness of breath or difficulty breathing
- Chest pain, especially when coughing or breathing deeply
- Fatigue and weakness
- Nausea, vomiting, or diarrhea (less common)
If pneumonia is suspected, a healthcare provider will conduct a physical examination, which may include listening to the lungs with a stethoscope, and may order diagnostic tests such as chest X-rays, blood tests, or sputum cultures.
Treatment Options
Treatment for pneumonia depends on the type and severity of the infection:
- Bacterial Pneumonia: Antibiotics are the primary treatment for bacterial pneumonia. It’s important to complete the full course of antibiotics even if symptoms improve to ensure the infection is fully eradicated.
- Viral Pneumonia: Antiviral medications may be prescribed for certain viral infections, but often, treatment focuses on supportive care, including rest, hydration, and over-the-counter medications to relieve symptoms.
- Fungal Pneumonia: Antifungal medications are used to treat fungal pneumonia, and the specific drug depends on the type of fungus causing the infection.
- Supportive Care: For all types of pneumonia, supportive care is essential. This includes staying hydrated, getting plenty of rest, using humidifiers to ease breathing, and taking pain relievers or fever reducers as needed.
In severe cases, hospitalization may be required, where patients might receive oxygen therapy, intravenous fluids, and other supportive treatments.
Conclusion
Pneumonia is a potentially serious condition that can be contracted at home through various means, including person-to-person transmission, environmental exposure, and aspiration. Recognizing the risk factors and implementing preventive measures can significantly reduce the likelihood of developing pneumonia. Vaccinations, good hygiene practices, maintaining a healthy lifestyle, and ensuring a clean and well-ventilated home environment are all crucial in preventing pneumonia. Early detection and appropriate treatment are key to a full recovery and minimizing complications. By staying informed and vigilant, individuals can protect themselves and their loved ones from this potentially life-threatening infection.
FAQ on Pneumonia
Can you catch pneumonia from someone who has it?
Yes, pneumonia can be contagious, depending on the cause. Bacterial and viral pneumonia can spread from person to person through airborne droplets from coughing or sneezing. However, not everyone who is exposed will develop pneumonia; some may develop milder respiratory infections.
Signs that pneumonia is improving
Signs that pneumonia is improving include:
- Reduced fever
- Decreased chest pain and discomfort
- Improved breathing and less shortness of breath
- Increased energy and activity levels
- Decreased coughing and mucus production
Is pneumonia deadly?
Pneumonia can be deadly, particularly for certain populations, including the elderly, infants, and people with weakened immune systems or chronic health conditions. Prompt medical treatment is crucial to manage symptoms and complications.
What not to do when you have pneumonia
When you have pneumonia, avoid:
- Smoking, as it can further irritate your lungs
- Staying inactive; gentle movement can help clear your lungs, but avoid strenuous activity
- Ignoring symptoms or delaying medical treatment
- Avoiding prescribed medications; complete the full course of antibiotics if prescribed
- Staying dehydrated; drink plenty of fluids to help loosen mucus in your lungs
Symptoms of pneumonia in adults
Common symptoms of pneumonia in adults include:
- Cough, often with phlegm
- Fever, which can be mild or high
- Chills and sweating
- Shortness of breath
- Chest pain that worsens with breathing or coughing
- Fatigue and muscle aches
- Confusion, particularly in older adults
How is pneumonia spread?
Pneumonia is typically spread through:
- Airborne droplets from coughing or sneezing
- Direct contact with an infected person or contaminated surfaces
- Inhalation of airborne particles containing pathogens
- Aspiration of bacteria from the mouth or throat into the lungs
Causes of pneumonia in adults
Pneumonia in adults can be caused by:
- Bacteria: Streptococcus pneumoniae is the most common cause.
- Viruses: Influenza, respiratory syncytial virus (RSV), and SARS-CoV-2 (COVID-19).
- Fungi: More common in individuals with weakened immune systems.
- Mycoplasma: Atypical pneumonia caused by Mycoplasma pneumoniae.
- Aspiration: Inhaling food, drink, vomit, or saliva into the lungs.